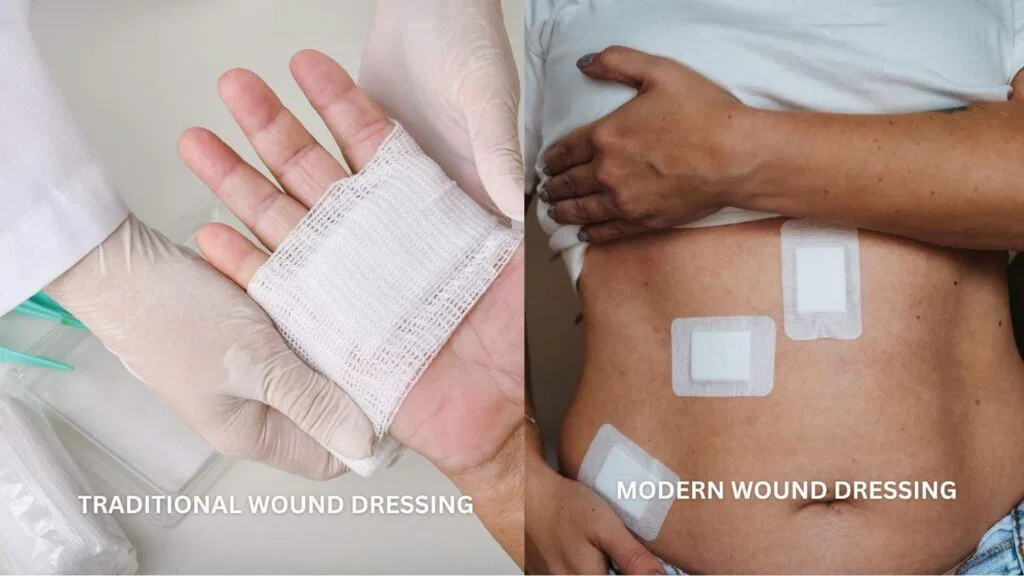
Comparing Traditional vs. Modern Wound Dressing Materials
Dry. Irritated. Stuck.
That gauze pad hurts to peel off.
It’s itchy. Red. The skin tears a little.
Then there’s the smell. And the drainage. You clean it. Wrap it again.
Tomorrow, the same.
If this sounds familiar—you’re not alone. Traditional dressings like gauze have been around for ages. And in some cases, they still serve a purpose. But many wounds today especially chronic or complex ones—need more advanced care.
Modern wound dressings do more than just cover. They hydrate. Protect. Soothe. Some even fight bacteria.
A recent study published by the NIH supports what many wound care clinicians already know: moist wound healing, often provided by modern dressings, speeds recovery and reduces pain.
And Johns Hopkins Medicine emphasizes the importance of choosing the right dressing based on wound characteristics—not just habit.
At OWC Center, we blend science and empathy to choose what’s right for your unique skin.
Let’s explore the most common wound dressing types—from classic gauze to advanced foams and hydrocolloids—and what they mean for healing.
Understanding Gauze in Wound Care
When people think of wound care, gauze is often the first thing that comes to mind. It’s been around for generations—tucked into every first-aid kit, stocked in every pharmacy, and used in everything from scraped knees to surgical incisions. But in today’s world of advanced wound healing, is gauze still the best option?
What Gauze Does Well
Gauze is inexpensive, accessible, and incredibly versatile. It’s ideal for:
- Dry wounds or minor abrasions: It provides a clean protective layer without adding extra moisture.
- Layering or custom sizes: Gauze can be folded, cut, or wrapped to fit just about any wound area.
- Airflow: Unlike some occlusive dressings, gauze allows the wound to breathe, which can be beneficial for certain surface injuries.
Because of its flexibility, gauze still plays a useful role in wound care—but it’s often most effective when used as part of a more comprehensive dressing system.
The Limitations of Gauze
While gauze has its strengths, it also comes with significant limitations—especially for complex or chronic wounds. These include:
- Sticking to the wound bed: When gauze dries out, it can adhere to healing tissue. This not only causes pain during dressing changes but can also damage the delicate granulating tissue that’s essential for healing.
- Frequent dressing changes: Gauze often needs to be changed more than once a day, which can increase patient discomfort, interrupt the healing process, and expose the wound to potential contamination.
- Inadequate moisture balance: One of the most important advancements in modern wound care is the understanding that wounds heal best in a moist environment. Gauze does not retain moisture well, which can slow down healing—especially for pressure injuries or post-surgical sites.
In short, while gauze can be helpful in early or superficial wounds, it may not provide the optimal healing environment for deeper, draining, or more fragile wounds.
Gauze in Practice at OWC Center
At OWC Center, we use gauze thoughtfully and selectively. It’s often applied as a secondary dressing to secure a primary antimicrobial or moisture-balancing layer in place. For instance:
- Padding for compression bandages in vascular ulcers
- Temporary covers while awaiting lab results or further evaluation
- Supportive dressing over more advanced materials like hydrocolloids or foams
We also use non-adherent versions of gauze when appropriate, to reduce the risk of trauma during dressing changes—especially in patients with diabetes, vascular complications, or sensitive skin.
However, for patients with complex wounds, such as diabetic foot ulcers, pressure injuries, or wounds with excessive drainage, gauze often isn’t enough. These cases require more advanced wound care technologies that are designed to promote faster healing, control infection, and minimize patient discomfort.
Benefits of Hydrocolloids for Healing
When it comes to modern wound healing, hydrocolloid dressings are among the most trusted tools in advanced wound care. These dressings are designed to do more than just cover a wound—they actively create a healing environment that’s comfortable, protective, and ideal for skin regeneration.
So, what exactly makes hydrocolloids different?
Hydrocolloids are made of gel-forming agents (like pectin or gelatin) combined with a flexible outer layer. When placed over a wound, they interact with the wound fluid to form a soft, moist gel that helps tissues repair and regenerate naturally—without the dryness or irritation that older dressings often cause.
Key Benefits of Hydrocolloid Dressings
- Promote moist healing without sticking
Unlike gauze, hydrocolloids don’t stick to the wound bed. This allows new tissue to grow undisturbed and makes dressing changes far more comfortable for patients. - Reduce dressing change frequency
Many hydrocolloid dressings can stay in place for several days—sometimes up to a week depending on the wound and its drainage. Fewer changes mean less disruption to healing, lower risk of contamination, and more convenience for patients. - Provide gentle insulation
These dressings help regulate temperature and protect against external bacteria or friction, offering a cushioning effect that’s especially helpful for pressure-prone areas. - Excellent for pressure injuries and non-infected ulcers
Hydrocolloids are commonly used for stage I or II pressure ulcers, shallow wounds, donor sites, and low-exudate surgical wounds. Their flexibility makes them a favorite choice for areas like the sacrum or heels.
Hydrocolloids in Action at OWC Center
At OWC Center, hydrocolloids are often part of our protocol for treating pressure injuries, skin tears, and early-stage ulcers, particularly in elderly patients or those with fragile skin. Their ability to conform to the body and support healing with minimal intervention makes them a go-to choice when comfort and moisture control are essential.
Patients appreciate that these dressings are low-profile and discreet, and our team values their reliability in reducing wound pain and supporting natural healing without constant interference.
Hydrocolloids may not be suitable for infected or heavily draining wounds—but for the right wound, they can make all the difference.
👉 Explore our Pressure Injury Treatment approach
When Not to Use Hydrocolloids
- Infected or heavily draining wounds
- Highly exudative ulcers
Anecdote:
One of our patients with a shallow sacral pressure ulcer saw significant healing progress with hydrocolloid therapy—no painful removal, fewer dressing changes, and visibly improved skin within two weeks.
Why Foam Dressings Are a Game Changer
Foam dressings offer versatility and comfort, especially for wounds with moderate to heavy drainage.
Foam Dressings Excel In:
- Absorbing excess exudate
- Protecting high-friction areas (heels, hips)
- Providing cushioning for painful wounds
- Supporting faster epithelial growth
5 Common Uses for Foam Dressings:
- Diabetic foot ulcers
- Surgical incisions
- Venous leg ulcers
- Trauma wounds
- Post-debridement care
Story from the Clinic:
A patient with a diabetic foot wound reported less pain and better mobility after transitioning from gauze to a self-adherent foam dressing—allowing them to stay active and confident in their recovery.
👉 Discover our Diabetic Foot Ulcer Treatment strategy
Choosing the Right Wound Dressing Type
Every wound is unique—and so is every healing journey.
What We Consider When Recommending Dressings
- Type of wound (surgical, traumatic, chronic)
- Drainage level
- Location and skin sensitivity
- Infection risk or comorbidities
At OWC Center, we combine clinical assessment with compassion to recommend the best dressing type. Whether it’s hydrocolloids for a fragile bed sore, foam for a diabetic ulcer, or gauze as a temporary barrier, your care is always personalized.
👉 Schedule your personalized Wound Assessment today
Not all wounds need the same kind of attention—and that starts with the dressing you choose. While gauze may be familiar and widely used, it’s not always enough for complex wounds or those that require moisture control and comfort. Today’s advanced options like hydrocolloids and foam dressings bring more than just coverage; they actively create healing environments that protect, cushion, and accelerate recovery.
At OWC Center, we don’t just treat the surface—we look deeper. By understanding the type of wound, how it behaves, and what your body needs to heal, we’re able to match you with the right tools from the very beginning. Whether you’re caring for a pressure injury, diabetic ulcer, or post-surgical wound, modern dressing materials—when chosen thoughtfully—can make all the difference in healing faster and feeling better.
Key Takeaways
- Not all dressings are created equal—choose based on the wound, not routine.
While gauze has its place, many wounds benefit more from advanced materials like foam or hydrocolloids. These modern options support healing by maintaining moisture, reducing pain, and preventing infection. - Gauze is best used as support—not the main solution.
Dry wounds or low-drainage injuries may respond well to gauze, especially when used as a secondary dressing. But for complex or draining wounds, gauze alone may slow healing or cause discomfort. - Hydrocolloids offer gentle, consistent healing for shallow wounds.
These gel-based dressings seal and protect wounds while promoting tissue regeneration. They’re especially helpful for pressure ulcers or fragile skin, reducing dressing changes and improving comfort. - Foam dressings are a go-to for diabetic and draining wounds.
Foam’s moisture-retaining and cushioning abilities make it ideal for wounds that need protection and absorption. From foot ulcers to surgical wounds, it supports both healing and comfort. - The right dressing starts with a proper assessment.
Every wound is different. At OWC Center, we begin with a full evaluation to choose the most effective dressing—whether it’s gauze, hydrocolloid, foam, or a hybrid approach—tailored to your healing needs.
5 Related Questions Asked and Answered
1. What are the main differences between traditional and modern wound dressing types?
Wound dressings have come a long way from simple gauze and tape. While traditional materials like gauze are still used, modern dressings are designed to support healing in more advanced ways.
Traditional Dressings:
- Often dry or absorbent materials like plain gauze or cotton pads
- Primarily protect the wound and absorb fluids
- Require frequent changing and can stick to the wound, causing discomfort
Modern Dressings:
- Include hydrocolloids, foams, alginates, and silicone-based materials
- Maintain moisture balance to support tissue regeneration
- Offer antimicrobial protection, promote pain-free removal, and reduce scarring
At OWC Center, we assess each wound’s depth, moisture level, and risk of infection to recommend the most appropriate dressing—whether it’s a simple gauze pad or an advanced multi-layer foam.
2. When is gauze still useful in wound care?
Gauze is one of the oldest and most accessible wound care materials—and it still has a role to play. However, it’s best suited for specific situations and used in combination with other dressings.
Gauze dressings are most appropriate when:
- The wound is dry or has minimal drainage
- The dressing needs to be changed frequently
- It’s being used as a secondary dressing to secure medication or padding
However, gauze can be problematic if used on wounds with heavy drainage or if it sticks to the wound bed, which may slow healing and cause pain during removal. Modern wound management often supplements gauze with hydrogels or non-adherent layers to avoid complications.
At OWC Center, we consider gauze a supportive tool—not the go-to for every wound.
3. What are hydrocolloid dressings, and when are they recommended?
Hydrocolloids are gel-forming dressings that promote a moist healing environment and protect against contaminants. They’re flexible, skin-friendly, and excellent for wounds that aren’t heavily draining.
Benefits of hydrocolloids:
- Create a sealed, insulated environment for optimal healing
- Minimize the need for frequent dressing changes
- Reduce pain during removal
- Useful for pressure ulcers, shallow wounds, or early-stage bed sores
They may not be ideal for infected wounds or those with excessive exudate. But for the right cases, hydrocolloids can significantly accelerate healing with fewer interruptions.
OWC Center often uses hydrocolloids as part of our pressure injury management protocols, especially for patients with fragile or aging skin.
👉 Read more about our Pressure Injury Treatment approach
4. How do foam dressings compare to traditional materials like gauze?
Foam dressings are a standout in modern wound care. Unlike gauze, which may dry out or stick to a wound, foam dressings offer cushioned, moisture-retaining support ideal for moderate to heavily draining wounds.
Advantages of foam dressings include:
- High absorbency for exudate
- Protection from pressure and friction
- Comfort for patients with sensitive skin or wounds in high-movement areas
- Compatibility with secondary antimicrobial agents if needed
They’re especially helpful for diabetic foot ulcers, post-surgical wounds, or trauma wounds where comfort and containment are key.
At OWC Center, we regularly use foam in combination with compression or antimicrobial therapy to accelerate healing and reduce complications.
5. How do you choose the right dressing for your wound?
Choosing the right dressing isn’t just about the material—it’s about the wound itself. Factors like depth, drainage, infection risk, and skin sensitivity all play a role in selection.
We typically assess:
- Wound type and depth (e.g., ulcer, laceration, surgical)
- Moisture level (dry vs. heavily draining)
- Signs of infection or inflammation
- Patient comfort and mobility needs
This is why the OWC Center begins every treatment with a comprehensive wound assessment. We match dressing types—whether gauze, hydrocolloids, foam, or a combination—to each individual’s condition and healing stage.
We don’t believe in a “one-size-fits-all” solution—because no two wounds (or patients) are alike.