Guidelines for Negative Pressure Wound Therapy
Negative pressure wound therapy (NPWT) has revolutionized wound care management. At Optimum Wound Care (OWC), we’ve seen firsthand how this innovative treatment accelerates healing and reduces complications for patients with complex wounds.
Our comprehensive guide to negative pressure wound therapy guidelines will equip healthcare professionals with essential knowledge and best practices. We’ll explore the principles behind NPWT, implementation techniques, and strategies for monitoring treatment progress.
Understanding Negative Pressure Wound Therapy (NPWT)
Definition and Basic Principles
Negative Pressure Wound Therapy (NPWT) revolutionizes wound care management. This advanced technique applies controlled negative pressure to a wound bed through a specialized dressing. NPWT creates a sealed environment that promotes healing by:
- Removing excess fluid and exudate
- Reducing edema
- Increasing blood flow to the wound area
- Stimulating granulation tissue formation
NPWT System Components
The NPWT system typically consists of three main components:
- Foam dressing (cut to fit the wound)
- Adhesive film
- Pump (generates negative pressure)
Healthcare professionals place the foam dressing directly on the wound bed. The adhesive film seals the wound and connects to the pump via tubing. When activated, the pump creates a vacuum effect, which draws out excess fluid and promotes a moist healing environment.
Efficacy and Benefits
Research supports the effectiveness of NPWT. A study found that NPWT is able to decrease infection treatment times and wound healing time compared to conventional wound treatment.
Suitable Wound Types
NPWT demonstrates versatility across various wound types, including:
- Diabetic foot ulcers
- Pressure ulcers
- Surgical wounds
- Traumatic wounds
- Venous leg ulcers
This therapy proves particularly effective for wounds that heal slowly or face high infection risks. However, healthcare providers must note that NPWT isn’t suitable for all wounds. Contraindications include exposed organs, untreated osteomyelitis, and malignancy in the wound bed.
Practical Implementation Guidelines
To implement NPWT effectively, healthcare professionals should follow these key guidelines:
- Conduct a thorough wound assessment: Evaluate the wound type, size, and location to ensure NPWT appropriateness.
- Prepare the wound bed properly: Debride necrotic tissue (when necessary) before NPWT application to ensure optimal results.
- Customize pressure settings: Start with a pressure of -125 mmHg (adjustable based on patient comfort and wound characteristics).
- Monitor regularly: Assess the wound at each dressing change (typically every 48-72 hours) to track progress and make necessary adjustments.
These guidelines help healthcare providers achieve impressive outcomes for patients, often resulting in faster healing times and improved quality of life.
As we move forward, let’s explore the best practices for implementing NPWT, including patient assessment, proper dressing application techniques, and pressure level settings.
Implementing NPWT: Best Practices
Patient and Wound Assessment
Effective implementation of Negative Pressure Wound Therapy (NPWT) starts with a comprehensive evaluation. Healthcare professionals should:
- Review patient history (underlying conditions, medications, previous treatments)
- Examine wound characteristics (size, depth, location, tissue type, exudate levels, infection signs)
- Check vascular status to ensure adequate blood supply
- Evaluate nutritional status and address any deficiencies
A study in the Journal of Wound Care reported that thorough initial assessments reduced treatment time for complex wounds by 30%.
Dressing Application Techniques
Proper dressing application is essential for NPWT success. Follow these steps:
- Clean the wound with saline or an appropriate antiseptic solution
- Remove any necrotic tissue if necessary
- Cut the foam dressing to fit the wound precisely (avoid overlap onto healthy skin)
- Apply a non-adherent layer to protect delicate structures if needed
- Seal the dressing with an occlusive drape (ensure a 3-5 cm border around the wound)
- Create a small opening in the drape for the suction pad
Negative pressure wound therapy (NPWT) promotes healing by evenly applying negative pressure on the surface of the wound.
Pressure Settings Optimization
Tailor pressure settings to each patient and wound type:
- Begin at -125 mmHg for most wounds
- Use lower pressures (-75 to -100 mmHg) for painful wounds or fragile tissue
- Consider higher pressures (up to -200 mmHg) for highly exudative wounds
- Adjust based on patient comfort and wound response
Tailored NPWT settings, based on the ANSWER score, may enhance wound healing outcomes in patients with microangiopathy. Further clinical studies are needed to confirm this approach.
Dressing Change Frequency
The frequency of dressing changes depends on several factors:
- Change dressings every 48-72 hours (typical interval)
- Increase frequency for infected wounds or high exudate levels
- Extend intervals up to 7 days for clean, progressing wounds
- Change immediately if there’s loss of seal or signs of infection
Optimizing dressing change frequency can reduce overall treatment costs by up to 20% while maintaining excellent outcomes.
Healthcare providers who follow these guidelines can maximize the potential of NPWT technology. The next section will explore strategies for monitoring NPWT progress and managing potential complications.
Monitoring and Managing NPWT Progress
Assessing Treatment Effectiveness
Healthcare professionals should look for specific indicators of successful NPWT:
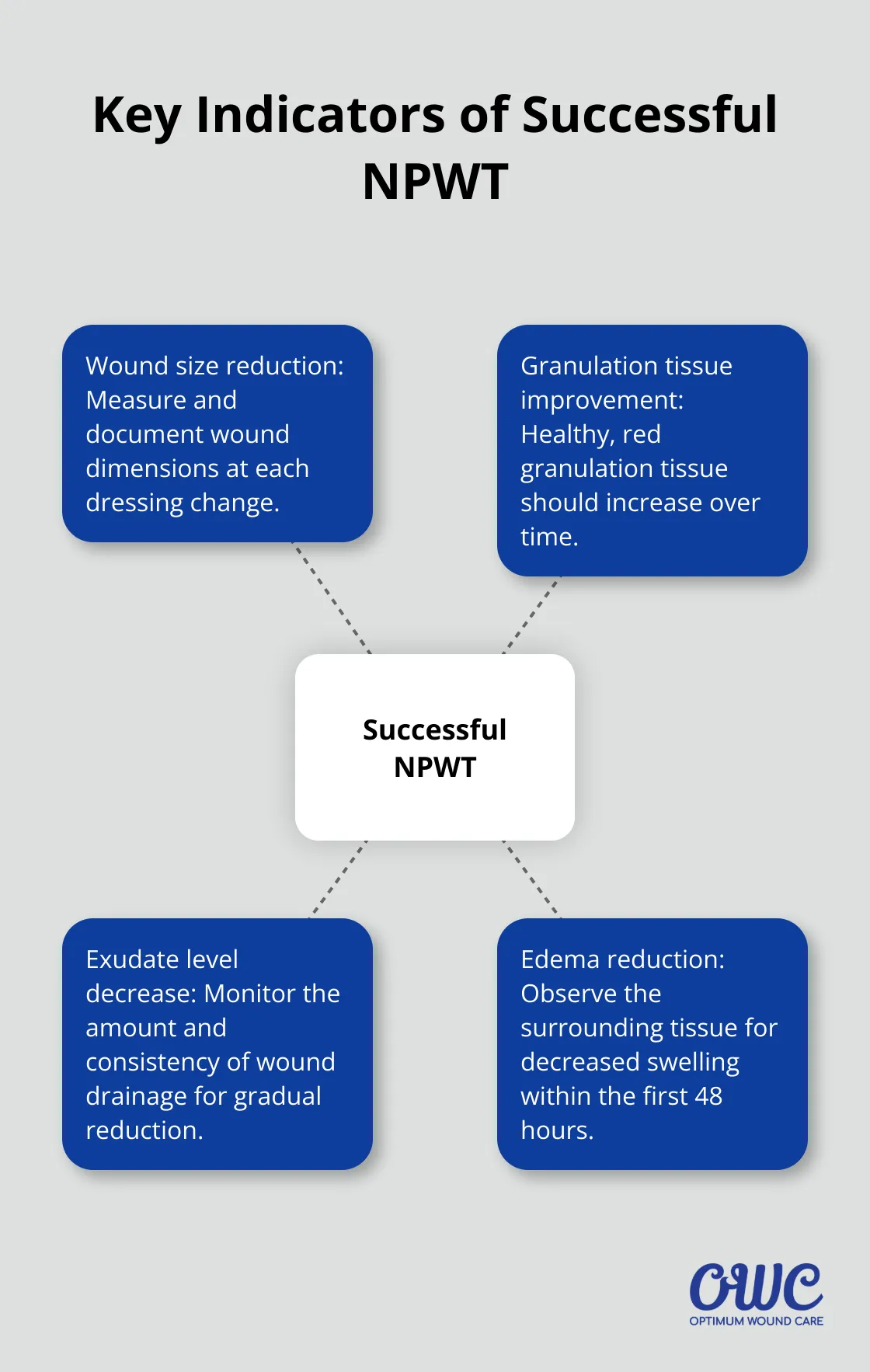
- Wound size reduction: Measure and document wound dimensions at each dressing change.
- Granulation tissue improvement: Healthy, red granulation tissue should increase over time. Wound VAC stimulates the formation of granulation tissue, which plays a vital role in wound healing.
- Exudate level decrease: Monitor the amount and consistency of wound drainage. A gradual reduction in exudate volume indicates progress.
- Edema reduction: Observe the surrounding tissue for decreased swelling, which often occurs within the first 48 hours of NPWT initiation.
Addressing Common Complications
NPWT is generally safe, but complications can arise. Here’s how to address common issues:
- Pain management: If patients report increased discomfort, adjust pressure settings or consider intermittent therapy.
- Infection control: Look for signs such as increased exudate, odor, or surrounding erythema. Increase dressing change frequency and consider adding antimicrobial dressings or systemic antibiotics as needed.
- Bleeding mitigation: Minor bleeding is common but should decrease over time. For persistent bleeding, reduce pressure or consider discontinuing therapy.
- Skin irritation prevention: Apply protective barriers around the wound edges and ensure the drape doesn’t overlap onto healthy skin.
Determining Treatment Duration
The decision to discontinue NPWT depends on several factors:
- Wound closure achievement: Stop when the wound bed is filled with granulation tissue and ready for secondary closure or skin grafting.
- Healing plateau identification: Reassess the treatment plan if no significant progress is observed after 2-3 weeks.
- Patient factor consideration: Discontinue if the patient experiences persistent pain or complications that outweigh benefits.
- Treatment goal attainment: Stop NPWT when specific objectives (e.g., infection control or exudate management) are achieved.
Early use of NPWT demonstrated better healing despite greater significant comorbidities in patients receiving this treatment.
Patient Education and Empowerment
Patient education is vital for NPWT success. Provide clear instructions on:
- Device operation: Teach patients how to operate the NPWT pump and troubleshoot common alarms.
- Dressing integrity maintenance: Instruct patients to check the seal daily and report any leaks immediately.
- Activity level guidance: Encourage mobility while avoiding activities that may disrupt the dressing.
- Warning sign recognition: Educate patients on when to seek medical attention (e.g., increased pain, fever, or excessive bleeding).
- Follow-up appointment adherence: Stress the importance of regular check-ups to monitor progress and adjust treatment as needed.
Final Thoughts
Negative pressure wound therapy guidelines have transformed wound care management. This innovative treatment accelerates healing, reduces complications, and improves patient outcomes across various wound types. Healthcare professionals must create individualized treatment plans, considering each patient’s unique needs, wound characteristics, and overall health status.
Continuous monitoring and adjustment are essential throughout the treatment process. Healthcare providers must watch for signs of progress or potential complications, adapting the therapy as needed. Patient education and empowerment ensure treatment adherence and early detection of issues.
Optimum Wound Care (OWC) provides expert wound care services and stays at the forefront of NPWT advancements. Our experienced clinical team combines cutting-edge techniques with compassionate care to help patients heal faster and regain their quality of life. We invite you to explore our services and experience the benefits of advanced wound care (tailored to your specific needs).

