Complications of Negative Pressure Wound Therapy
Negative pressure wound therapy (NPWT) has revolutionized wound care, but it’s not without risks. At Optimum Wound Care (OWC), we’ve seen firsthand how this treatment can accelerate healing for many patients.
However, understanding negative pressure wound therapy complications is crucial for healthcare providers and patients alike. This blog post will explore the potential issues that can arise during NPWT and provide practical strategies for prevention and management.
What is Negative Pressure Wound Therapy?
Negative Pressure Wound Therapy (NPWT) revolutionizes wound care. At Optimum Wound Care, we observe remarkable results with this technique, especially for patients with complex or slow-healing wounds.
NPWT applies controlled suction to a wound through a specialized dressing. This negative pressure extracts excess fluid and debris, promotes better blood flow, and encourages the formation of new tissue. It doesn’t just remove unwanted material; NPWT actively stimulates the wound bed, initiating the healing process.
The Science Behind NPWT
NPWT’s effectiveness stems from its ability to create an optimal healing environment. It maintains a moist wound bed and reduces bacterial load, addressing key factors that can impede healing. Studies have shown a reduction in healing time, recurrence rates, and postoperative pain, as well as higher patient satisfaction with the use of NPWT.
When to Use NPWT
We recommend NPWT for various wound types. It’s particularly effective for:

However, NPWT isn’t suitable for all wounds. Wounds with exposed organs, untreated osteomyelitis, or malignancy (contraindicated for this therapy) should not receive NPWT.
The NPWT Process
At Optimum Wound Care, we follow a strict protocol for NPWT application. First, we clean and debride the wound thoroughly. Then, we apply a specialized foam dressing cut to fit the wound precisely. This is covered with an airtight film, and a tube connects the dressing to the NPWT device.
The device creates negative pressure, with modern systems offering a range of pressure settings from -40mmHg to -200mmHg, depending on the wound type and patient tolerance. We usually change dressings every 48 to 72 hours, allowing us to monitor progress closely.
Patient Experience
While NPWT can significantly speed up healing, it presents challenges. Some patients report discomfort or pain, especially during dressing changes. We always prioritize patient comfort, adjusting pressure levels and providing pain management as needed.
NPWT requires commitment from both healthcare providers and patients. It’s not a set-it-and-forget-it solution. Regular follow-ups are essential, and patients need to stay vigilant about keeping the device functioning correctly.
Now that we understand what NPWT is and how it works, let’s explore the potential complications that can arise during this treatment. Understanding these risks is essential for both healthcare providers and patients to ensure safe and effective wound management.
Common Complications of Negative Pressure Wound Therapy
Negative Pressure Wound Therapy (NPWT) is a powerful tool in wound management, but it comes with potential risks. Understanding these complications is essential for healthcare providers and patients to ensure safe and effective treatment.
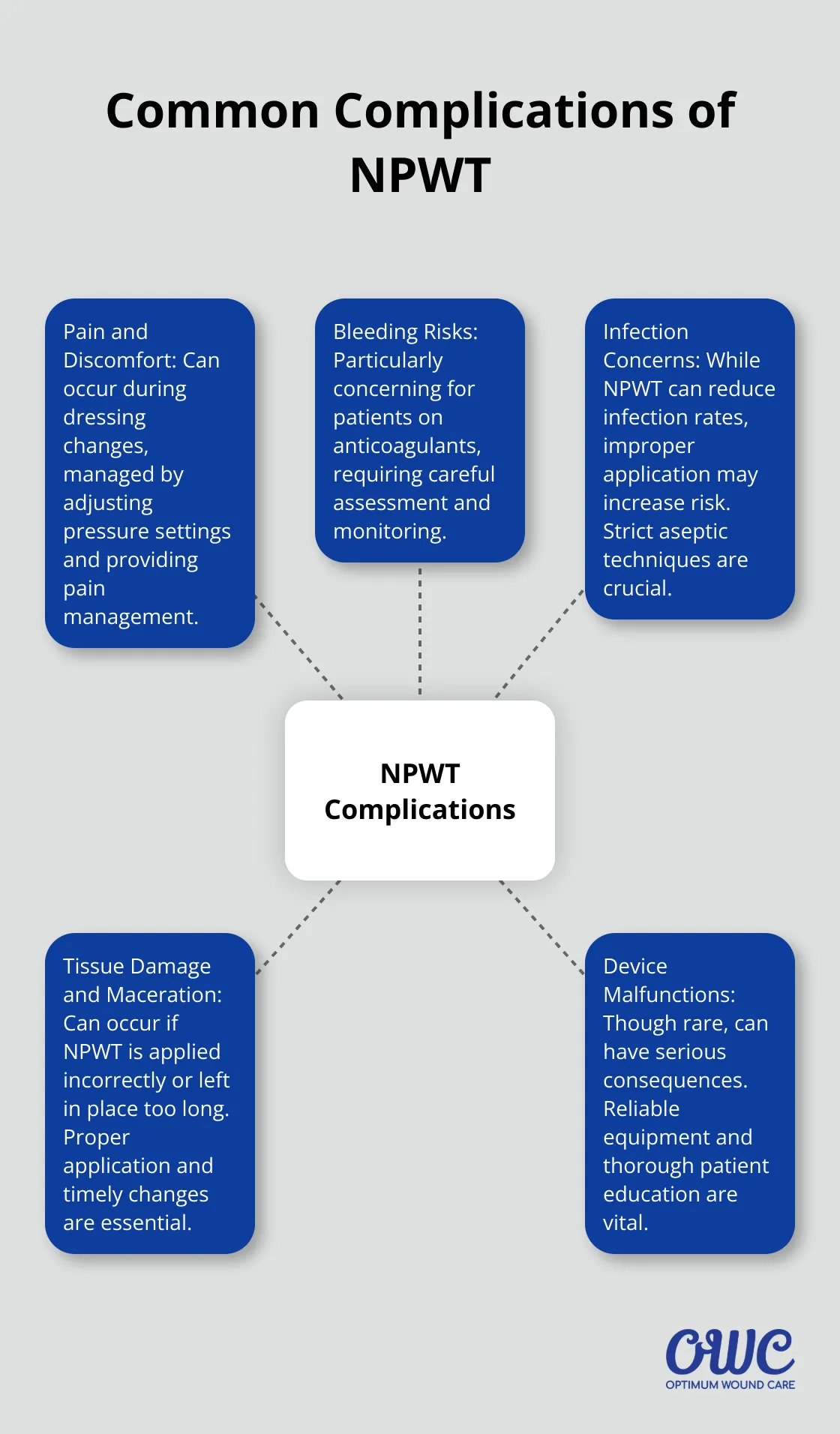
Pain and Discomfort
Pain during dressing changes is one of the issues patients face during NPWT. However, studies have shown that gauze-based NPWT can result in less pain during dressing changes. Healthcare providers address this by adjusting pressure settings and providing appropriate pain management strategies.
Bleeding Risks
Bleeding presents another concern, particularly in patients on anticoagulants. Manufacturers recommend caution when using NPWT in patients with active bleeding or those taking anticoagulants. Healthcare professionals carefully assess patients’ coagulation status before initiating therapy and monitor closely throughout treatment.
Infection Concerns
While NPWT can reduce infection rates, improper application may lead to the opposite effect. Healthcare providers maintain strict aseptic techniques during dressing changes and educate patients on recognizing signs of infection to mitigate this risk.
Tissue Damage and Maceration
Tissue necrosis and maceration can occur if NPWT is applied incorrectly or left in place for too long. Prevention involves ensuring proper dressing application and adhering to recommended change intervals.
Device Malfunctions
Device malfunctions, while rare, can have serious consequences. The FDA received reports of six deaths and 77 injuries associated with NPWT systems over a two-year period. Healthcare providers combat this by using reliable equipment and providing thorough patient education on device operation and troubleshooting.
Awareness of these complications serves as the foundation for effective prevention. Healthcare professionals implement rigorous protocols and maintain open communication with patients to maximize the benefits of NPWT while minimizing its risks. The next section will explore strategies to prevent and manage these complications, ensuring optimal outcomes for patients undergoing NPWT.
How to Prevent NPWT Complications
At Optimum Wound Care, we developed a comprehensive approach to minimize complications associated with Negative Pressure Wound Therapy (NPWT). Our strategy focuses on meticulous patient selection, precise application techniques, and ongoing monitoring to ensure optimal outcomes.
Patient Assessment
The foundation of successful NPWT lies in careful patient selection. We conduct thorough evaluations, considering factors such as wound type, size, and location, as well as the patient’s overall health status. Patients with untreated osteomyelitis or exposed blood vessels are not suitable candidates for NPWT. Our team uses advanced diagnostic tools to assess wound characteristics and underlying conditions, ensuring that NPWT is the most appropriate treatment option.
Application Techniques
Correct application of NPWT prevents complications. Our specialists follow a strict protocol that includes:

We use a checklist during the application process to reduce errors and improve consistency across our team.
Monitoring and Dressing Changes
Regular monitoring catches potential issues early. Our nurses perform daily checks on NPWT patients, looking for signs of infection, excessive bleeding, or device malfunction. We implemented a standardized assessment tool that helps us quantify wound progress and detect complications quickly.
Dressing changes are critical moments in NPWT treatment. We schedule these every 48 to 72 hours (depending on wound characteristics and exudate levels). During changes, we reassess the wound, adjust the therapy as needed, and ensure patient comfort throughout the process.
Patient and Caregiver Education
Education prevents NPWT complications. We provide comprehensive training to patients and their caregivers, covering topics such as:
- Recognition of infection signs or other complications
- Proper care and maintenance of the NPWT device
- When and how to seek medical attention
Our patients receive a detailed handbook and have access to a 24/7 helpline for immediate support.
Therapy Cessation
We established clear criteria for therapy cessation, including:
- Achievement of treatment goals (e.g., adequate granulation tissue formation)
- Lack of progress after two weeks of therapy
- Development of severe complications
These guidelines ensure that patients don’t undergo unnecessary treatment and reduce the risk of long-term complications.
Final Thoughts
Negative pressure wound therapy has transformed wound care, offering hope for patients with complex wounds. However, NPWT complications can occur, ranging from pain to serious issues like bleeding and infection. These risks highlight the importance of vigilant care and proper management throughout the treatment process.
At Optimum Wound Care (OWC), we prioritize patient safety and effective wound management. Our team at Optimum Wound Care combines clinical expertise with advanced techniques to deliver personalized treatment. We focus on patient education, regular monitoring, and precise application to minimize negative pressure wound therapy complications.
The future of NPWT promises even safer and more effective treatments. Ongoing research aims to improve device designs, enhance pressure control systems, and develop smart dressings (capable of detecting early signs of complications). These advancements will further reduce risks and maximize the benefits of NPWT for patients.