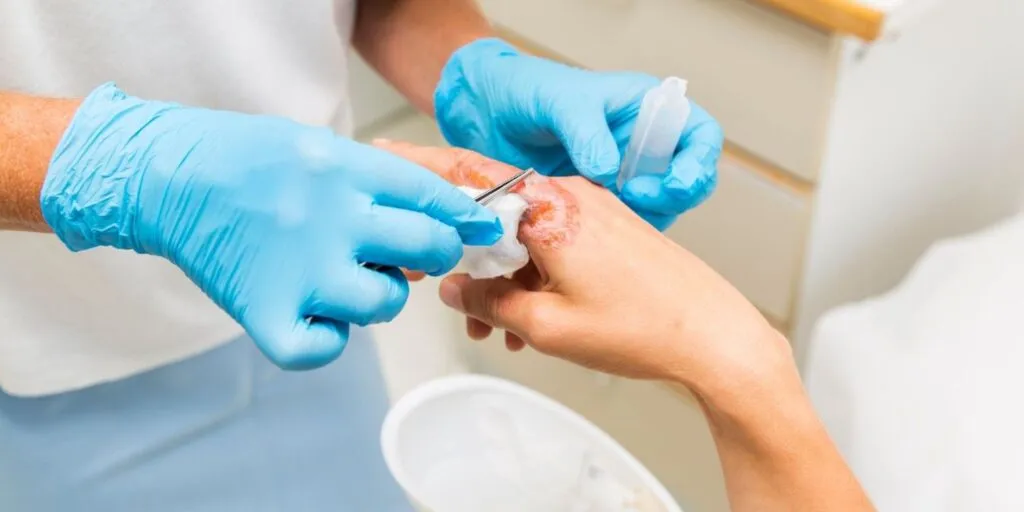
What to Know About Fungal Wound Infections
Open wound. Slow healing. Itchy. Red. Moist.
Something doesn’t feel right.
It looks like it might be infected. But not the usual kind. No pus. No yellow crust. Just this persistent irritation, sometimes a strange smell, and no signs of improvement.
You go to the drugstore. Try an antibiotic cream. Nothing changes. In fact, it gets worse.
This could be a fungal wound infection.
While most people think of bacteria when they hear the word “infection,” fungal infections are sneakier especially in open wounds. Fungi thrive in warm, damp environments, and if you’re dealing with diabetes, poor circulation, or a compromised immune system, your body may struggle to fight back.
According to research, fungal wound infections are becoming more common in people with chronic health conditions. These infections can slow recovery, increase pain, and even spread under the skin if not treated correctly.
At OWC Center, we understand the frustration of wounds that won’t heal. That’s why we look deeper. Beyond the surface. Beyond the usual.
Let’s explore the signs, risks, treatments, and preventions of fungal wound infections—because healing starts with understanding.
Skin Infections Can Be More Than Bacterial
Fungal wound infections are often overlooked because their symptoms mimic other common wound issues. However, they behave very differently from bacterial infections.
What Makes Fungal Skin Infections Unique?
- Appearance: They tend to present as red, inflamed, and itchy rather than swollen and pus-filled.
- Odor: May have a musty or sour smell, unlike the sharp odor from bacterial infections.
- Response to Treatment: Antibiotics do not work—and can even make fungal infections worse by disturbing the skin’s natural balance.
At OWC Center, we use precise wound assessment tools to detect fungal organisms, especially when a wound isn’t responding to traditional care.
If you’ve already tried over-the-counter antibiotics or seen no improvement with basic dressings, the issue might be fungal.
Common Skin Fungi
- Candida (especially in moist skin folds)
- Aspergillus (common in immunocompromised patients)
These microbes can enter wounds easily, especially when the skin barrier is compromised.
👉 Explore how our Advanced Wound Care goes beyond surface symptoms
Why Antifungal Treatment Must Be Personalized
No two wounds are alike—and neither are fungal infections. That’s why treatment at OWC Center is never one-size-fits-all.
Types of Antifungal Treatments We Use
- Topical antifungals
- For superficial infections or early-stage fungal growth
- Commonly prescribed creams include clotrimazole, miconazole, or nystatin
- Oral antifungals
- Needed when infections spread or resist topical agents
- Includes fluconazole or itraconazole
- Surgical debridement
- Removes infected tissue and biofilm buildup
- Advanced dressings
- Designed to wick away moisture and limit fungal growth
- Moisture control strategies
- Critical because fungi thrive in moist environments
Every wound we treat gets a full evaluation, sometimes including cultures or biopsies, to determine the correct antifungal approach.
External resource: CDC guide on fungal skin infections explains different types and prevention.
👉 Read more about wound care options at our Louisville clinic
Who Gets Fungal Wound Infections? (And Why It Matters)
Some people are more vulnerable. Knowing your risk can help you take action early.
High-Risk Groups Include:
- Diabetics with foot ulcers or neuropathy
- Cancer patients undergoing chemotherapy
- Elderly individuals with thin, fragile skin
- Those with compromised circulation or lymphedema
- Patients using corticosteroids or immunosuppressants
When combined with moisture or prolonged wound exposure, these factors make fungal growth much more likely.
If you fall into any of these categories and your wound hasn’t healed, you may need antifungal evaluation.
👉 Check out our Diabetic Foot Ulcer Treatment program
5 Quick Signs You May Need Antifungal Care:
- Itching that gets worse over time
- Rashes or red rings around the wound
- Discoloration or soft white patches
- Unusual odor from the wound site
- Little to no improvement with antibiotics
Don’t wait for symptoms to worsen. Early care leads to faster recovery.
Preventing Skin Infections That Turn Fungal
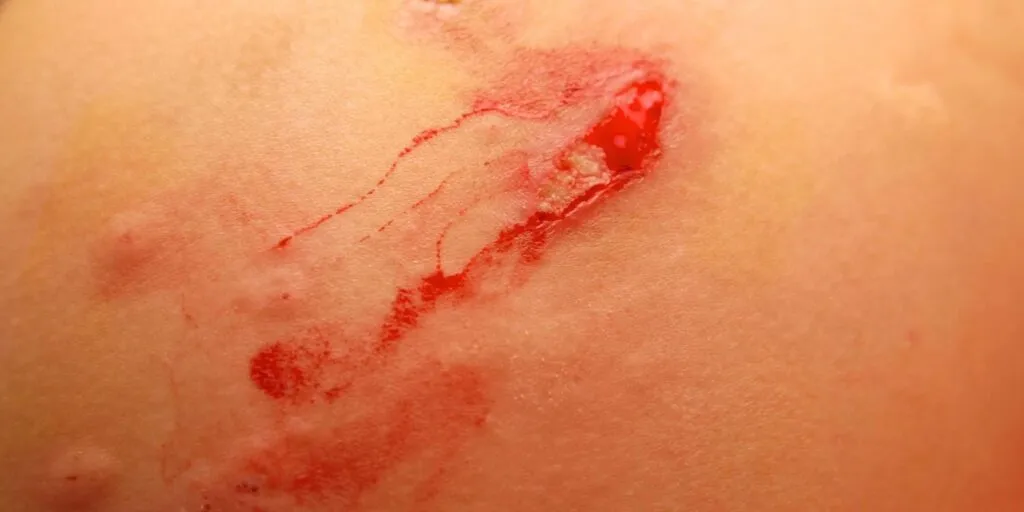
Fungal wound infections are treatable—but they’re even better when preventable.
Practical Prevention Tips
- Keep wounds clean and dry
- Avoid unnecessary antibiotic use
- Use breathable dressings to reduce trapped moisture
- Change dressings as directed by your provider
- Monitor for early signs like itchiness, odor, or color change
Incorporating these habits can make a huge difference, especially for those with chronic wounds or immune suppression.
Fungal wound infections may not always be the first thing we think of when a wound isn’t healing—but they’re more common, and more serious, than most people realize. Whether you’re dealing with diabetes, aging skin, immune challenges, or a history of antibiotic use, your skin is more vulnerable to fungal intrusion than you might think.
Subtle signs like itching, redness, a musty odor, or a wound that stubbornly refuses to heal shouldn’t be ignored. Unlike bacterial infections, these don’t respond to standard antibiotic creams. In fact, those treatments can sometimes make things worse.
The good news is, early recognition and the right antifungal approach can make a world of difference. From topical solutions to advanced moisture-balancing dressings and personalized care plans, OWC Center offers the tools and expertise to help your skin recover—and stay protected.
If your wound isn’t healing the way it should, it’s time to ask why. Because sometimes, the issue runs deeper than you think—and knowing the difference could be the first step toward lasting recovery.
Key Takeaways
- Fungal wound infections are often missed—but they matter.
Unlike bacterial infections, fungal ones may not present with obvious pus or swelling. Instead, look for persistent redness, itching, and a wound that doesn’t improve. If that sounds familiar, it’s time to consider a more advanced evaluation.
- Antibiotics won’t help—and may even make things worse.
If your wound hasn’t responded to traditional antibiotic creams, it could be fungal. Overuse of antibiotics can disrupt your skin’s natural balance, making fungal infections more likely.
- Personalized antifungal care is key to healing.
From prescription antifungal creams to oral medications and specialized dressings, every infection requires a customized plan. OWC Center tailors each treatment based on wound depth, patient history, and diagnostic findings.
- At-risk groups need extra support.
People with diabetes, cancer, aging skin, or circulation issues are especially vulnerable to fungal complications. Our team closely monitors these patients with proactive prevention and early intervention strategies.
- Prevention makes all the difference.
Keeping wounds clean, dry, and monitored is essential. At OWC Center, we don’t just treat—we teach. Our goal is to empower you with habits that protect your skin for the long haul.
5 Related Questions Asked and Answered
1. What exactly is a fungal wound infection?
Fungal wound infections occur when fungi—such as Candida or Aspergillus—infect open wounds. While not as common as bacterial infections, they can be serious, especially in individuals with weakened immune systems, diabetes, or chronic wounds.
Here’s what you need to know:
- Fungi thrive in warm, moist environments—making open wounds an ideal entry point if not cleaned and treated properly.
- Common causes include poor hygiene, immunosuppression (like in cancer or diabetes patients), or long-term antibiotic use (which can disrupt the skin’s natural flora).
- Symptoms often include increased redness, itching, unusual discharge, foul odor, or a wound that’s not healing as expected.
If you suspect a fungal wound infection, don’t delay—these infections can spread quickly beneath the skin surface. OWC Center specializes in diagnosing and treating skin infections of all types, including fungal cases that resist over-the-counter solutions.
👉 Learn more about our Advanced Wound Care services.
2. How do fungal wound infections differ from bacterial ones?
It’s a great question—and an important distinction. Many people assume all infected wounds are bacterial, but fungal infections behave quite differently.
Key differences include:
- Cause: Bacterial infections stem from pathogens like Staphylococcus or Streptococcus, while fungal infections often involve Candida or environmental molds.
- Appearance: Fungal infections may look more inflamed or itchy rather than pus-filled or crusted like bacterial ones.
- Response to antibiotics: Antibiotics won’t help fungal infections—in fact, they may worsen them by disrupting the skin’s natural balance.
- Treatment needs: Fungal infections require antifungal treatment, often in the form of topical creams or oral medication, depending on severity.
At OWC Center, our multidisciplinary wound care team uses wound assessment tools to identify the exact cause of infection and prescribe effective solutions tailored to your body’s needs.
3. Who is most at risk for fungal wound infections?
Anyone with an open wound can develop a fungal infection, but certain groups are more vulnerable. Understanding these risk factors can help you protect yourself or a loved one from complications.
High-risk groups include:
- Diabetic patients – particularly those with foot ulcers or neuropathy
- Elderly individuals – due to thinner skin and slower healing
- Cancer patients or those on chemotherapy – because of weakened immunity
- People using long-term antibiotics or corticosteroids
- Those with poor circulation or lymphedema
If you or someone you care for falls into one of these categories, it’s essential to work with a clinic experienced in managing chronic wound infections—like OWC Center in Louisville. We monitor for signs of fungal growth as part of every wound care plan.
4. What are the most effective treatments for fungal wound infections?
Treating fungal wound infections requires a precise, evidence-based approach. At OWC Center, we use a combination of therapies to target the infection while supporting the healing of surrounding skin tissue.
Common treatments include:
- Topical antifungals: Creams or ointments applied directly to the infected area
- Oral antifungals: Used when topical options aren’t effective or if the infection spreads
- Wound debridement: Removing dead or infected tissue to prevent further fungal growth
- Moisture control: Fungi love moist environments, so maintaining a balanced wound environment is crucial
- Customized wound dressings: Designed to both treat infection and support faster recovery
Every treatment plan at OWC Center is customized after a thorough wound assessment. Early intervention leads to better outcomes and fewer complications.
5. Can fungal wound infections be prevented?
Absolutely! Prevention is a major part of our care philosophy at OWC Center. While not every fungal infection can be avoided, taking proactive steps greatly reduces the risk.
Tips for prevention:
- Keep wounds clean and dry
- Avoid overuse of antibiotics (which can disrupt healthy skin flora)
- Use breathable dressings to manage moisture
- Change dressings regularly as instructed by your care provider
- Watch for early warning signs like redness, itching, or discharge
If you have underlying conditions such as diabetes or vascular issues, regular checkups and wound monitoring are essential. At OWC Center, we believe in empowering patients with knowledge and preventive strategies for lifelong skin and wound health.