What’s the Best Way to Treat Bed Sores at Home or in a Facility?
Bed sores can be a painful and serious complication for those with limited mobility.
This guide will explore effective bed sore treatment options, from basic home care techniques to advanced medical interventions. We’ll provide practical advice to help you or your loved ones prevent and manage bed sores effectively.
Understanding Bed Sores: Causes, Stages, and Risk Factors
What Are Bed Sores?
Bed sores (also known as pressure ulcers or decubitus ulcers) are areas of damaged skin and tissue caused by sustained pressure that reduces blood flow to vulnerable areas of the body. Patients with limited mobility or those confined to beds or wheelchairs for extended periods often develop these painful wounds.
The Four Stages of Bed Sores
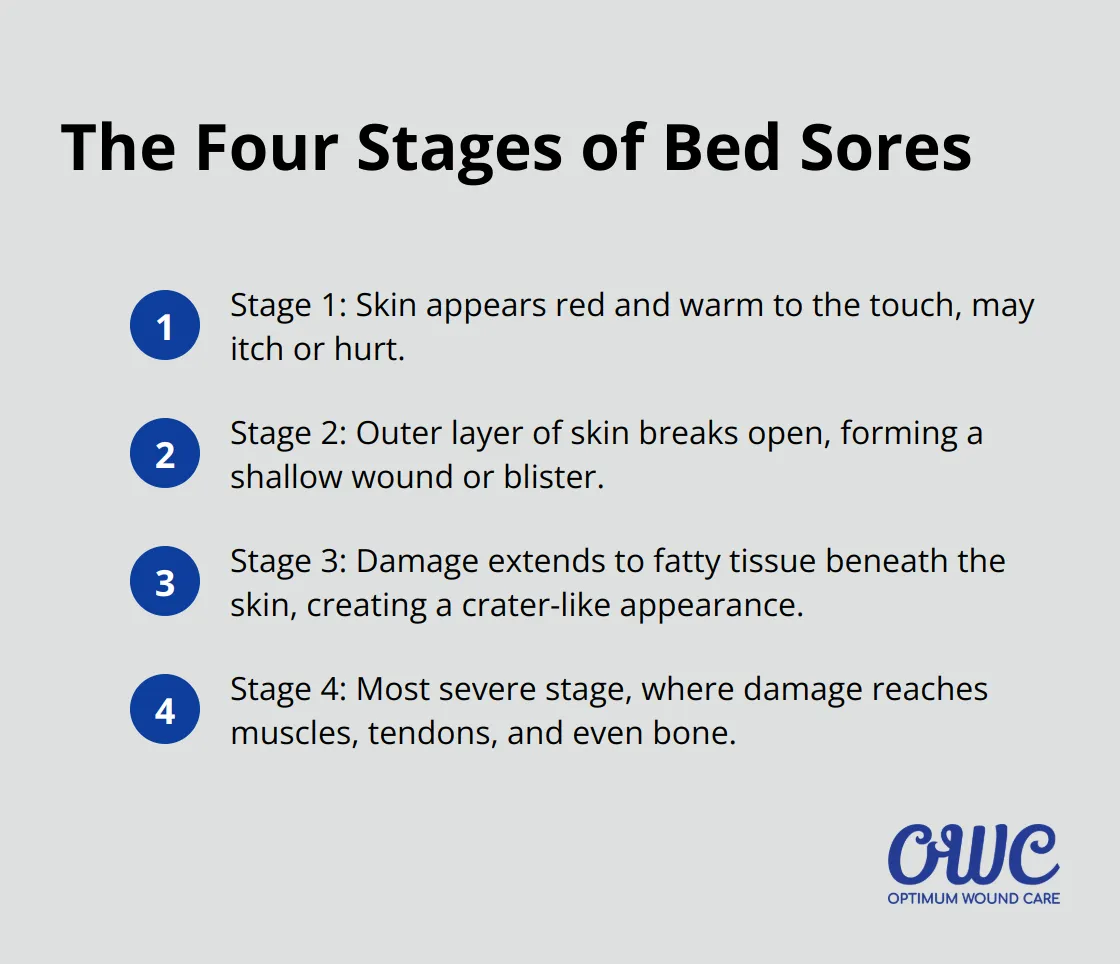
Bed sores progress through four distinct stages:
- Stage 1: The skin appears red and warm to the touch. It may itch or hurt.
- Stage 2: The outer layer of skin breaks open, forming a shallow wound or blister.
- Stage 3: The damage extends to the fatty tissue beneath the skin, creating a crater-like appearance.
- Stage 4: The most severe stage, where damage reaches muscles, tendons, and even bone.
Early detection can prevent minor skin irritations from becoming severe wounds. Contact a healthcare provider immediately if you notice any persistent redness or discomfort in pressure-prone areas.
Risk Factors for Bed Sores
Several factors increase the likelihood of developing bed sores:
- Immobility: The primary cause (whether due to injury, illness, or sedation).
- Poor nutrition: Inadequate protein, vitamins, and minerals hinder wound healing.
- Moisture: Excessive sweat or incontinence can weaken skin integrity.
- Age: Older adults have thinner, less elastic skin, making them more susceptible.
- Medical conditions: Diabetes, vascular diseases, and spinal cord injuries can impair circulation and sensation.
High-Risk Body Areas
Certain parts of the body are more prone to bed sores due to their bony prominences:
- Tailbone and buttocks
- Heels and ankles
- Hips and lower back
- Shoulder blades and elbows
- Back of the head and ears
For wheelchair users, the shoulder blades, spine, and backs of arms and legs are particularly vulnerable.
Prevention Strategies
Prevention is always better than cure. Key strategies to avoid bed sores include:
- Frequent repositioning (every 2 hours for bedridden patients)
- Proper nutrition (high in protein, vitamins, and minerals)
- Maintaining clean, dry skin
Regular skin checks are essential, focusing on high-risk areas. Use a mirror or ask a caregiver to inspect hard-to-see spots. Early detection can prevent minor skin irritations from progressing to severe wounds.
If you’re concerned about bed sores or need expert wound care, don’t hesitate to reach out to a healthcare professional. Optimum Wound Care, for instance, offers specialized services to help patients heal faster and improve their quality of life. In the next section, we’ll explore effective home treatment methods for managing bed sores.
How to Treat Bed Sores at Home
Repositioning for Pressure Relief
Frequent repositioning forms the foundation of bed sore prevention and treatment. For bedridden patients, change positions regularly. Alternate between the back, sides, and stomach if possible. Use pillows to support the body and alleviate pressure on vulnerable areas. When repositioning, lift rather than drag the person to avoid friction damage.
Wheelchair users should shift their weight regularly. The “wheelchair push-up” technique proves effective: patients use arm strength to lift their body off the seat for a short period. If the person can’t perform this independently, caregivers must assist with regular position changes.
Selecting Appropriate Support Surfaces
Specialized mattresses and cushions play a vital role in bed sore treatment. Reactive air surfaces may reduce the chances of developing new ulcers compared with foam surfaces. These surfaces have shown promising results in managing pressure ulcers.
For less severe cases, alternating pressure mattresses or foam overlays can effectively distribute weight more evenly and reduce pressure on vulnerable areas. When selecting a support surface, consult with a healthcare provider to ensure it meets the specific needs of the patient.
Wound Care Techniques
Proper cleaning and dressing of bed sores promotes healing and prevents infection. Follow these steps:
- Wash hands thoroughly and wear clean gloves.
- Clean the wound gently with saline solution or mild soap and water.
- Pat the area dry with a clean towel.
- Apply any prescribed topical treatments.
- Cover the wound with an appropriate dressing (hydrocolloid dressings for stages 1 and 2, alginate dressings for more advanced wounds).

Change dressings at least daily, or more often if they become soiled. Always inspect the wound during dressing changes and report any signs of infection (increased redness, warmth, swelling, or foul odor) to a healthcare provider immediately.
Nutrition for Wound Healing
Proper nutrition accelerates the healing process. A diet rich in protein, vitamins A and C, and zinc supports wound healing. Increased needs for energy, protein, zinc, and Vitamins A, C, and E, as well as amino acids, are important for wound healing.
Hydration plays an equally important role. Ensure the patient drinks adequate water daily (unless contraindicated by other health conditions). Adequate hydration supports skin elasticity and overall healing.
While these home treatment methods prove effective for many bed sores, always consult with a healthcare professional for proper diagnosis and treatment planning, especially for more advanced wounds. Early intervention and consistent care prevent complications and promote faster healing. In the next section, we’ll explore professional treatment options available in healthcare facilities for more severe cases of bed sores.
Advanced Wound Care in Healthcare Facilities
Debridement: Removing Dead Tissue
Debridement removes dead or infected tissue from a wound to promote healing. Healthcare providers use various methods:
- Surgical debridement: A surgeon removes dead tissue with scalpels or sharp instruments. This method works fast and effectively for large or deep wounds.
- Enzymatic debridement: Special enzymes break down dead tissue. This gentler approach suits patients who cannot tolerate surgical procedures.
- Autolytic debridement: The body’s natural enzymes dissolve dead tissue. This method uses specialized dressings to keep the wound moist, supporting the body’s healing process.
The choice of debridement method depends on wound severity, patient health, and provider expertise.
Negative Pressure Wound Therapy: Speeding Up Healing
Negative Pressure Wound Therapy (NPWT) transforms the treatment of severe bed sores. This technique applies controlled negative pressure to the wound area using a vacuum-assisted closure device. NPWT offers several benefits:
- Removes excess fluid and reduces swelling
- Increases blood flow to the wound
- Promotes granulation tissue formation
- Reduces infection risk
A study found that NPWT may speed up the reduction of pressure ulcer size and severity, reduce pain, and decrease dressing change times compared to usual care. However, NPWT doesn’t suit all patients (particularly those with bleeding disorders or untreated infections).
Surgical Interventions for Severe Cases
Stage 3 or 4 bed sores may require surgical intervention. These procedures close the wound, prevent infection, and restore function to the affected area. Common surgical options include:
- Skin grafts: Surgeons transplant healthy skin from another body part to cover the wound.
- Flap surgery: A section of skin, muscle, and blood vessels moves from a nearby area to cover and protect the wound.
- Direct closure: For smaller wounds, surgeons may close the wound by bringing the edges together.
It is estimated that 1 to 2 percent of the population in developed countries will suffer from a chronic wound in their lifetime. These procedures carry risks and require careful patient selection and post-operative care.
Advanced Treatment Options at Specialized Clinics
Specialized wound care clinics offer a range of advanced treatments for severe bed sores. For instance, Optimum Wound Care combines clinical expertise with state-of-the-art techniques to provide personalized care. Their experienced team, led by Wound/Ostomy Specialist Mosayeb “Moe” Karimi, MSN, FNP, WOC, tailors their approach to ensure the best possible outcomes for each unique patient situation.
Healthcare providers typically reserve these advanced treatments for severe cases or when conservative measures fail. The decision to pursue these options should always involve consultation with a healthcare provider, considering the patient’s overall health, wound characteristics, and potential risks and benefits of each approach.
Final Thoughts
Bed sore treatment requires a multifaceted approach that combines early intervention, consistent care, and professional medical guidance. The key to successful management lies in prevention and prompt action at the first signs of skin damage. Regular repositioning, proper nutrition, and maintaining clean, dry skin form the foundation of effective bed sore prevention and treatment.
Home care plays a vital role in managing bed sores, but patients must balance it with professional medical advice. Some cases may require advanced treatments only available in healthcare facilities, so regular consultations with healthcare providers ensure that treatment strategies evolve with the changing needs of the wound and the patient’s overall health status. Long-term management of bed sores involves ongoing vigilance and adaptability as wounds heal or new challenges arise.
For those who seek specialized care for complex wounds, Optimum Wound Care offers comprehensive services tailored to individual patient needs. Their team of experts combines clinical knowledge with state-of-the-art techniques to promote faster healing and improved quality of life. The right combination of home care, professional guidance, and advanced treatments (when necessary) can help patients effectively manage bed sores and maintain a good quality of life.

