How to Provide Nursing Care for Negative Pressure Wounds
At Optimum Wound Care (OWC), we understand the importance of effective wound care in nursing practice. Negative pressure wound therapy (NPWT) has revolutionized the treatment of complex wounds, offering faster healing and reduced complications.
This guide will walk you through the essential steps of negative pressure wound therapy nursing care, from patient assessment to dressing changes. We’ll cover best practices, troubleshooting tips, and the latest developments in NPWT to help you provide top-notch care for your patients.
Understanding Negative Pressure Wound Therapy (NPWT)
The Mechanics of NPWT
Negative Pressure Wound Therapy (NPWT) revolutionizes wound care treatment. This innovative approach uses controlled suction to promote healing in complex wounds. NPWT applies sub-atmospheric pressure to the wound bed through a specialized dressing. This negative pressure removes excess fluid, reduces edema, and increases blood flow to the wound. The result? Faster formation of granulation tissue and quicker wound closure.
A typical NPWT system includes:
- A foam or gauze dressing
- An airtight drape
- Tubing connected to a suction pump
- A collection canister for wound drainage
The pressure settings range from -40 mmHg to -200 mmHg, depending on the wound type and patient tolerance. Wound care specialists carefully select the appropriate pressure for each unique case.
Suitable Candidates for NPWT
NPWT isn’t a universal solution. It proves most effective for:
- Diabetic foot ulcers
- Pressure ulcers
- Surgical wounds
- Traumatic wounds
- Skin grafts
However, NPWT is contraindicated in cases of untreated osteomyelitis, exposed blood vessels, or malignancy in the wound bed. Specialists always perform a thorough assessment before recommending NPWT.
NPWT’s Impact on Wound Healing
The benefits of NPWT are significant and well-documented. NPWT can:
- Accelerate wound closure
- Reduce the risk of infection
- Minimize the need for frequent dressing changes
- Improve patient comfort and mobility
Patients often report less pain and a quicker return to daily activities when using NPWT compared to traditional wound dressings.
Recent Advancements in NPWT
The field of NPWT continues to evolve. Recent innovations include portable, disposable NPWT devices that allow for greater patient mobility and home-based care. These advancements have made NPWT more accessible and cost-effective.
Another exciting development is the use of NPWT with instillation (NPWTi). This technique involves the periodic instillation of a solution (such as saline or an antimicrobial agent) into the wound bed before applying negative pressure. Early studies suggest that NPWTi may be particularly effective for infected wounds, with reductions in bacterial numbers of 46% in pressure ulcers, 22% in chronic wounds, and 56% in other wound types.

As we move forward, it’s important to consider how these advancements in NPWT technology can be applied in various clinical settings. The next section will explore the practical aspects of preparing for NPWT application, including patient assessment and equipment selection.
How to Prepare for NPWT Application
Comprehensive Patient Assessment
At Optimum Wound Care, we prioritize thorough patient evaluation before initiating Negative Pressure Wound Therapy (NPWT). Review the patient’s medical history, focusing on factors that may affect wound healing (such as diabetes, vascular disease, or immunosuppression).
Evaluate the wound itself. Measure its dimensions, assess the wound bed, and document the type and amount of exudate. The Wound, Ostomy and Continence Nurses Society recommends standardized assessment tools like the Bates-Jensen Wound Assessment Tool for consistent documentation.
Assess the periwound area. Look for signs of infection, maceration, or skin breakdown. These factors can significantly impact the success of NPWT.
Selecting the Right Equipment
Choose the appropriate NPWT system based on wound type, location, and exudate level. A portable NPWT device might suit ambulatory patients better, while a larger, more powerful unit may work better for heavily exudating wounds.
Ensure you have all necessary supplies on hand:
- Foam or gauze dressing
- Adhesive drape
- Suction tubing
- Collection canister
- Sterile saline for wound cleansing
- Protective skin barrier wipes
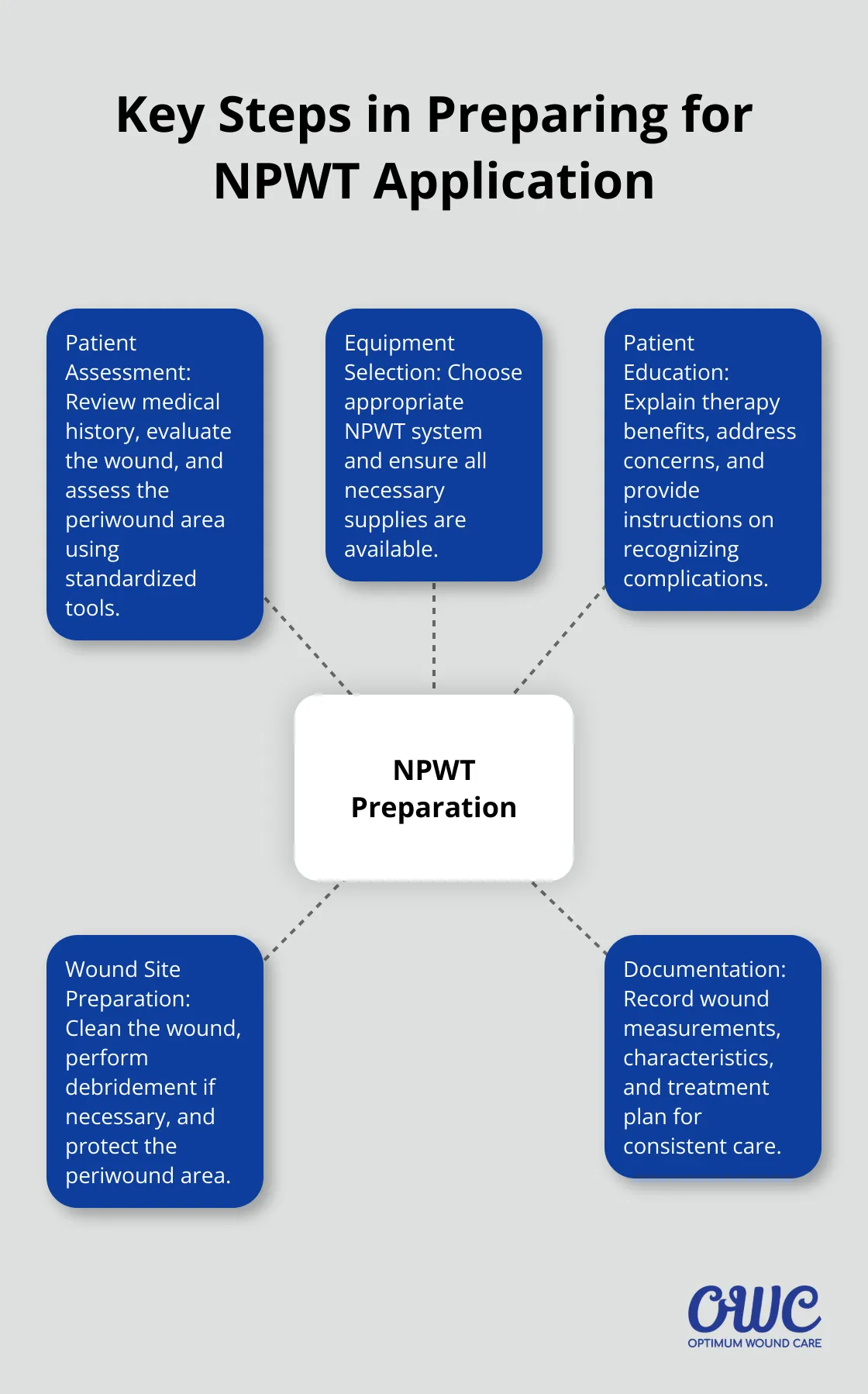
Patient Education for Compliance
Educate your patient about NPWT to ensure treatment success. Explain the therapy in simple terms, emphasizing its benefits and what to expect during treatment. Address any concerns or misconceptions they may have.
Teach patients how to recognize signs of complications (such as increased pain, redness, or fever). Provide clear instructions on when to contact healthcare providers.
If using a portable NPWT device, ensure the patient understands how to manage it at home.
Preparing the Wound Site
Clean the wound thoroughly with sterile saline or an appropriate wound cleanser. Remove any necrotic tissue through debridement if necessary. Dry the surrounding skin completely to ensure proper adhesion of the NPWT dressing.
Apply a skin barrier product to the periwound area to protect it from moisture and potential irritation from the adhesive drape. This step can help reduce the risk of skin complications during NPWT.
With these preparation steps complete, you’re ready to move on to the actual application of NPWT. The next chapter will guide you through the step-by-step process of applying and maintaining NPWT, ensuring optimal wound healing outcomes for your patients.
Mastering NPWT Application and Maintenance
At Optimum Wound Care, we have refined our approach to NPWT application and maintenance. Our process ensures optimal healing outcomes while minimizing complications. Here’s our expert guide to mastering NPWT:
Precise Dressing Application
Cut the foam dressing to fit the wound bed exactly. Avoid overlapping onto healthy skin to prevent maceration. For deep wounds, layer the foam to ensure complete wound contact.
Apply the adhesive drape, extending at least 5 cm beyond the wound edges. Create a 2 cm opening in the drape over the foam for the suction port. Attach the port and connect it to the NPWT device.
Initiate suction gradually, starting at -50 mmHg and increasing to the prescribed level. Observe the dressing to ensure it contracts and forms a seal.
Vigilant Monitoring and Adjustment
Check the NPWT system every 2-4 hours initially, then at least daily. Look for:
- Proper seal maintenance
- Adequate suction (listen for any air leaks)
- Appropriate exudate collection
- Signs of infection or tissue damage
Document wound appearance, exudate amount, and any patient discomfort at each check. Adjust therapy settings as needed based on wound progress and patient tolerance.
Proactive Troubleshooting
Common NPWT issues include:
- Loss of seal: Clean the area, apply additional drape, and consider using a stoma paste for difficult areas.
- Excessive bleeding: Stop therapy immediately and apply direct pressure. Notify the physician.
- Pain during therapy: Reduce pressure settings or consider intermittent therapy.
- Foam adherence: Use non-adherent dressings between the wound bed and foam.
Proactive troubleshooting significantly reduces therapy interruptions and improves patient outcomes.
Strategic Dressing Changes:
Change NPWT dressings every 2-3 days (or sooner if the canister fills rapidly). Follow these steps:
- Turn off suction and wait 15-30 minutes for foam to decompress.
- Remove the drape and foam gently, irrigating if necessary to ease removal.
- Assess the wound bed, measuring and documenting any changes.
- Clean the wound with sterile saline or prescribed cleanser.
- Reapply new foam, drape, and suction as described earlier.

During dressing changes, reassess the need for NPWT. Try transitioning to conventional dressings when granulation tissue fills 80% of the wound bed or weekly wound volume decrease is less than 15%.
These guidelines will maximize the benefits of NPWT for your patients. Each wound is unique, and therapy should be tailored to individual patient needs (considering factors such as wound type, location, and patient comfort).
Final Thoughts
Negative pressure wound therapy nursing care transforms complex wound management. We at Swell Country witness improved healing rates and patient outcomes through precise application and diligent monitoring. Our approach combines thorough assessments, meticulous dressing techniques, and proactive troubleshooting to maximize NPWT benefits.
Patient education and collaboration enhance therapy success. We prioritize clear communication about NPWT processes and expectations, empowering patients to actively participate in their care. This patient-centered philosophy aligns with our commitment to clinical excellence and compassionate treatment at Swell Country.
NPWT continues to evolve with portable devices and innovative techniques (such as instillation therapy). Healthcare providers must stay informed about these advancements to offer optimal care. For comprehensive wound care solutions and expert guidance on NPWT, visit OWC Center to explore our services and resources.