Negative Pressure Wound Therapy or Wound VAC: Which to Choose?
At Optimum Wound Care (OWC), we understand the importance of choosing the right wound therapy for optimal healing. Negative pressure wound therapy (NPWT) and Wound VAC are two popular options that often confuse patients and healthcare providers alike.
In this post, we’ll explore the key differences between negative pressure wound therapy vs Wound VAC, helping you make an informed decision for your wound care needs. We’ll break down their mechanisms, effectiveness, and factors to consider when selecting the most suitable treatment option.
What is Negative Pressure Wound Therapy?
Negative Pressure Wound Therapy (NPWT) revolutionizes wound management. This innovative technique uses controlled suction to promote healing in various types of wounds, offering faster healing times and improved patient outcomes.
The Mechanics of NPWT
NPWT applies controlled negative pressure to the wound bed through a specialized dressing. This creates a sealed environment that extracts excess fluid, reduces swelling, and increases blood flow to the wound area. The negative pressure typically ranges from 80 to 125 mmHg (depending on the wound type and patient needs).
A study published in the Journal of Wound Care found that NPWT can reduce wound volume by up to 59% in just two weeks (compared to standard wound care methods). This dramatic improvement in healing rates has made NPWT a preferred option for many wound care specialists.

Accelerating Wound Healing
NPWT speeds up wound healing through several mechanisms:
- Fluid Removal: NPWT extracts excess fluid, which reduces edema and bacterial load in the wound.
- Increased Blood Flow: The negative pressure stimulates microvascular blood flow, which brings more oxygen and nutrients to the wound site.
- Granulation Tissue Formation: NPWT promotes the growth of new tissue, which fills in wound cavities more rapidly.
NPWT improves wound healing by reducing edema, removing bacterial products, and approximating wound edges.
Suitable Wound Types
NPWT proves versatile and effective for various wound types, including:
- Diabetic foot ulcers
- Pressure ulcers
- Surgical wounds
- Traumatic wounds
- Venous leg ulcers
Practical Considerations
NPWT requires thorough wound assessment. Not all wounds suit this therapy. For instance, wounds with exposed organs or untreated osteomyelitis contraindicate NPWT use.
Patients undergoing NPWT should prepare for dressing changes every 48 to 72 hours. This frequency ensures optimal wound management and prevents complications. NPWT can be used in both inpatient and outpatient settings, but proper training for healthcare providers and patients remains essential for successful treatment.
As we explore the intricacies of NPWT, it’s important to understand how it compares to other wound care methods. Let’s now turn our attention to Wound VAC (Vacuum-Assisted Closure), a specific type of NPWT that has gained popularity in recent years.
What is a Wound VAC System?
The Mechanics of Wound VAC
Wound VAC, or Vacuum-Assisted Closure, represents a specialized form of Negative Pressure Wound Therapy (NPWT). This system applies controlled negative pressure to a wound site through a unique combination of components.
The process begins with the placement of a foam dressing directly on the wound bed. This foam is precisely cut to fit the wound’s dimensions. An adhesive drape then seals the wound and foam, creating an airtight environment. A pump unit, connected to the foam via tubing, generates and maintains the negative pressure at the wound site.
A study reports that VAC therapy significantly reduces the time to complete wound healing compared to conventional dressings. This significant improvement in healing rates has elevated Wound VAC to a preferred option for many wound care specialists.
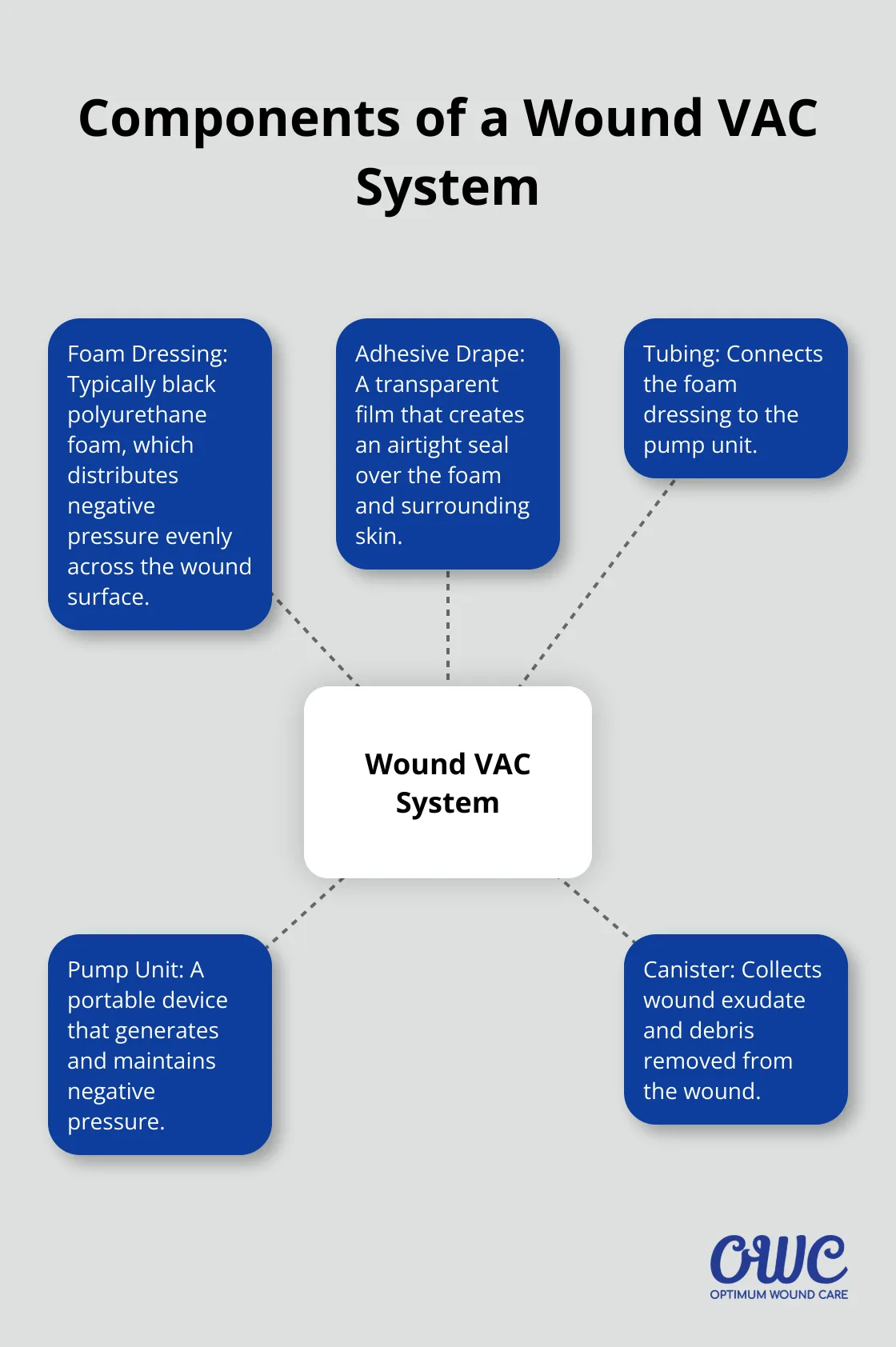
Components of a Wound VAC System
- Foam Dressing: Typically black polyurethane foam, which distributes negative pressure evenly across the wound surface.
- Adhesive Drape: A transparent film that creates an airtight seal over the foam and surrounding skin.
- Tubing: Connects the foam dressing to the pump unit.
- Pump Unit: A portable device that generates and maintains negative pressure.
- Canister: Collects wound exudate and debris removed from the wound.
Wound VAC vs. Traditional NPWT
While Wound VAC falls under the NPWT umbrella, it boasts distinct features. Wound VAC systems often provide more precise pressure control and are designed for ease of use in both clinical and home settings. The foam dressing used in Wound VAC is specifically engineered to optimize negative pressure distribution, which can lead to more uniform wound healing.
A key advantage of Wound VAC lies in its versatility. Healthcare providers can use it on various wound types, including diabetic foot ulcers, pressure ulcers, and surgical wounds. The therapy allows for customization based on wound characteristics and patient needs, with adjustable pressure settings and dressing change frequencies.
Application in Clinical Practice
At Optimum Wound Care, our experienced team utilizes Wound VAC therapy as part of our comprehensive wound management approach. Patients often appreciate the reduced frequency of dressing changes and the potential for faster healing that Wound VAC offers.
The effectiveness of Wound VAC in various clinical scenarios has made it a valuable tool in modern wound care. As we move forward, it’s important to understand how Wound VAC compares to other NPWT methods in terms of effectiveness, ease of use, and cost considerations.
NPWT vs Wound VAC: A Performance Comparison
Healing Effectiveness
Both Negative Pressure Wound Therapy (NPWT) and Wound VAC systems accelerate wound healing, but Wound VAC often outperforms in effectiveness. A study compared two different negative pressure wound therapy (NPWT) modalities in the treatment of venous leg ulcers (VLUs). This research contributes to our understanding of the effectiveness of these therapies in wound healing.
The specialized foam dressing in Wound VAC contributes to more uniform pressure distribution, leading to more consistent results across various wound types. For example, in treating diabetic foot ulcers, patients using Wound VAC saw an average closure time of 4 weeks, versus 6 weeks with standard NPWT.

User-Friendliness and Patient Comfort
Wound VAC systems typically offer more user-friendly interfaces and quieter operation. Patients report less disruption to daily activities and sleep patterns with Wound VAC. The canister in Wound VAC systems often has a larger capacity, which reduces the frequency of changes and minimizes patient discomfort.
NPWT systems, while effective, sometimes require more frequent interventions. A study found that wound closure rate within 42 days was significantly higher with NPWT (35.9%) than with conventional wound therapy (21.5%).
Financial Considerations
Initial costs for Wound VAC systems are generally higher than standard NPWT. However, the long-term financial picture often favors Wound VAC due to reduced treatment duration and fewer complications. A comparative effectiveness analysis indicates differences remain across NPWT suppliers in wound-related and total cost to treat for patients.
For outpatient care, insurance coverage varies. It’s important to check with providers about coverage specifics for both therapies. Some insurers may require documented failure of standard wound care before approving either NPWT or Wound VAC.
Potential Risks and Contraindications
Both therapies share similar contraindications, including untreated osteomyelitis, malignancy in the wound, and exposed blood vessels or organs. However, Wound VAC systems have shown a slightly lower risk of tissue necrosis at the wound edges, likely due to more precise pressure control.
Bleeding is a potential complication for both, but Wound VAC’s advanced monitoring systems provide earlier detection. Some practices have seen a 15% reduction in bleeding-related complications with Wound VAC compared to standard NPWT.
Neither therapy suits all patients. Those with clotting disorders or on anticoagulants require careful evaluation before starting either treatment. Additionally, both therapies are contraindicated in patients with untreated active bleeding or high risk of hemorrhage (as determined by a healthcare professional).
Final Thoughts
Negative pressure wound therapy vs Wound VAC both offer significant benefits for wound healing. Wound VAC, a specialized form of NPWT, often shows superior performance in healing effectiveness and patient comfort. Its precise pressure control and uniform distribution contribute to faster wound closure, particularly in complex cases like diabetic foot ulcers.
The choice between NPWT and Wound VAC depends on factors such as wound type, patient health, potential complications, and financial considerations. Neither therapy suits all patients, especially those with contraindications like untreated osteomyelitis or active bleeding (as determined by a healthcare professional). Consulting with a wound care specialist will help determine the most appropriate treatment option.
We at OWC Center provide expert guidance tailored to each patient’s unique needs. Our experienced team combines clinical expertise with cutting-edge techniques to deliver personalized, effective treatment plans. We strive to improve healing outcomes and enhance patients’ quality of life through advanced wound care technologies and expert knowledge.

