Does Negative Pressure Therapy Really Help Wounds Heal Faster?
At OWC Center, we’re often asked about innovative wound healing techniques. Negative pressure therapy has gained significant attention in recent years for its potential to accelerate wound healing.
This advanced treatment method uses controlled suction to promote tissue regeneration and reduce infection risk. In this post, we’ll explore the science behind negative pressure therapy and its effectiveness in wound management.
What Is Negative Pressure Wound Therapy?
Negative Pressure Wound Therapy (NPWT) revolutionizes wound care. At Optimum Wound Care, we witness how this innovative approach accelerates healing for our patients.
NPWT applies controlled suction to create negative pressure on a wound. This isn’t a simple vacuum – it’s a precisely calibrated system that applies the right amount of pressure to promote healing without causing damage.
How NPWT Accelerates Healing
NPWT creates an optimal environment for wound healing through several mechanisms:
- Excess Fluid Removal: NPWT suctions away excess fluid, which reduces swelling and bacterial growth.
- Blood Flow Enhancement: The negative pressure stimulates circulation to the wound area. This increases oxygen and nutrient delivery to healing tissues.
- Granulation Tissue Promotion: NPWT encourages new tissue formation.
Suitable Wound Types for NPWT
NPWT proves effective for various wound types:

- Diabetic Foot Ulcers: NPWT can be effective in treating neuroischemic ulcers when combined with best-practice standard care.
- Pressure Ulcers
- Surgical Wounds
- Traumatic Wounds: In cases of severe injury, NPWT prepares wounds for skin grafts or flaps more quickly than conventional methods.
Practical NPWT Tips
Consider these key points for NPWT success:
- Wound Bed Preparation: The wound requires thorough cleaning and debridement before NPWT application.
- Dressing Changes: Changes typically occur every 48-72 hours (less frequent than many traditional dressings).
- Pain Management: Many patients report less pain with NPWT compared to conventional dressings.
- Contraindications: NPWT isn’t suitable for wounds with exposed organs, untreated osteomyelitis, or malignancy in the wound bed.
At Optimum Wound Care, we integrate NPWT into our comprehensive wound management strategies. We find it particularly effective when combined with other advanced therapies like specialized dressings and bioengineered skin substitutes.
NPWT represents a significant advance in wound care technology. While it’s not a universal solution for all wounds, it can dramatically speed up healing and improve outcomes for many patients.
Now that we understand the basics of NPWT, let’s explore the scientific evidence supporting its efficacy in more detail.
Scientific Evidence Supporting NPWT Efficacy
Clinical Studies Reveal Promising Results
Research strongly supports the effectiveness of Negative Pressure Wound Therapy (NPWT). A comprehensive meta-analysis published in 2023 examined the use of incisional negative pressure wound therapy for the prevention of surgical site infection. The results were remarkable: NPWT has significant advantages in preventing postoperative wound infections compared to conventional treatment methods.
NPWT Outperforms Traditional Methods
When comparing NPWT to conventional dressings, the differences are significant. A study found that VAC therapy significantly decreases the time to complete wound healing, hastens granulation tissue formation, and reduces the ulcer area compared to conventional dressings.
Benefits for Specific Wound Types
NPWT demonstrates varying degrees of effectiveness depending on the wound type:
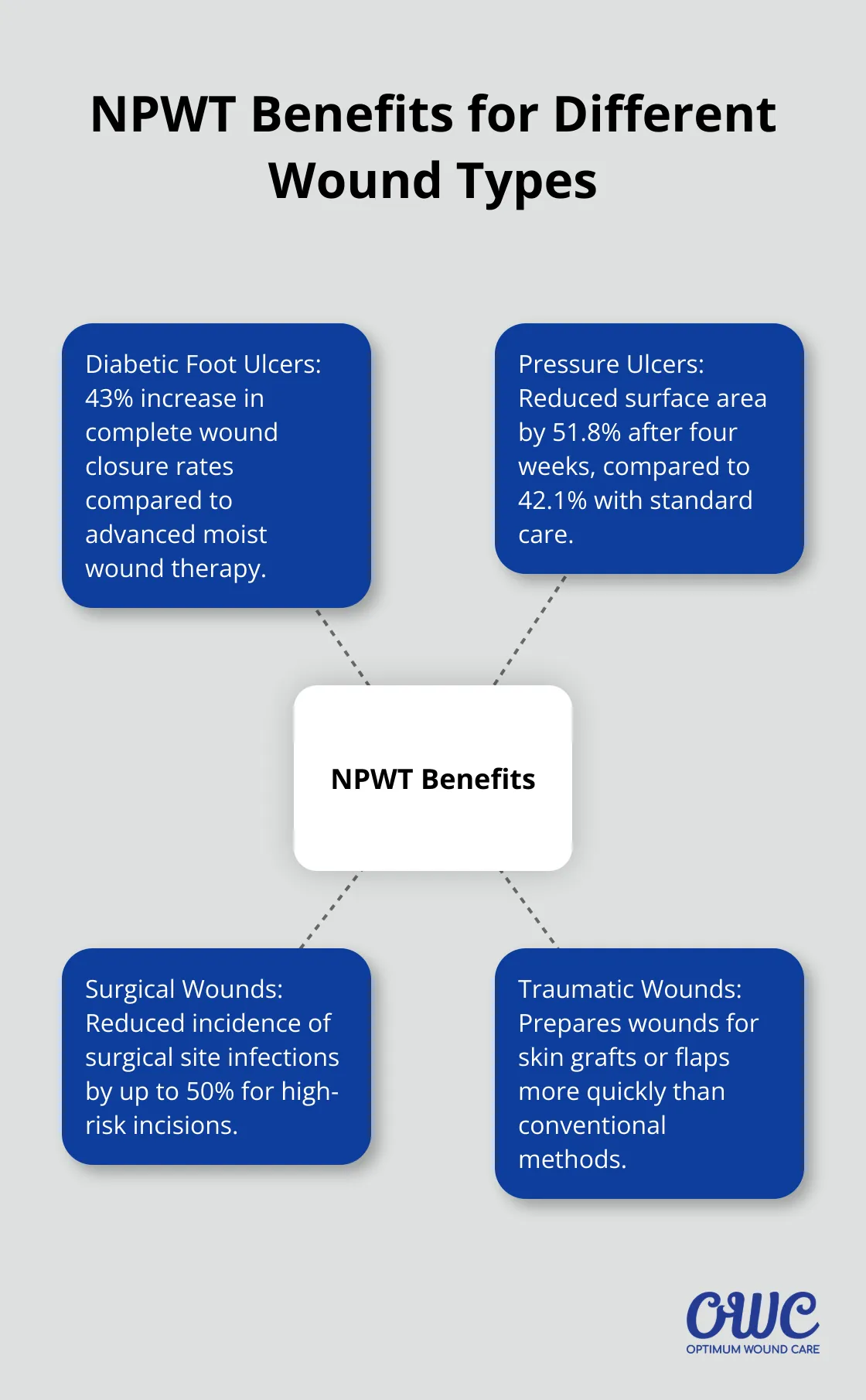
Diabetic Foot Ulcers
A randomized controlled trial published in Diabetes Care reported a 43% increase in complete wound closure rates for diabetic foot ulcers treated with NPWT compared to advanced moist wound therapy.
Pressure Ulcers
The Journal of Wound, Ostomy and Continence Nursing published a study showing that NPWT reduced the surface area of pressure ulcers by an average of 51.8% after four weeks of treatment, compared to 42.1% with standard care.
Surgical Wounds
For high-risk surgical incisions, NPWT has shown to reduce the incidence of surgical site infections by up to 50% (according to a study in the Annals of Surgery).
Real-World Application
At Optimum Wound Care, we’ve observed these benefits firsthand. Our patients consistently report faster healing times and improved comfort with NPWT. However, it’s important to note that every wound is unique, and treatment plans should be tailored to individual patient needs.
The evidence strongly supports NPWT’s effectiveness, but it’s not a universal solution. In the next section, we’ll explore practical considerations for using NPWT, including patient selection criteria and potential complications (which are essential factors in determining the most appropriate treatment approach).
Practical Considerations for NPWT Use
Patient Selection Criteria
Negative Pressure Wound Therapy (NPWT) proves most effective for specific patient groups. Ideal candidates include those with chronic, non-healing wounds that have not responded to conventional treatments. This encompasses diabetic foot ulcers, pressure ulcers, and surgical wounds that fail to close. Patients with adequate blood flow to the wound area and those who can tolerate pressure application typically benefit most from NPWT.
The therapy shows particular efficacy for individuals with large wounds or those at high risk of infection. NPWT is more superior in safety, cost-efficiency, and long-term wound management compared to standard wound care.
Contraindications and Precautions
NPWT is not recommended for all patients. Contraindications include:
- Untreated osteomyelitis
- Exposed blood vessels
- Malignancy in the wound bed
- Active bleeding
- Patients on anticoagulants
Individuals with fragile skin surrounding the wound or those with a history of adverse reactions to adhesive dressings may not be suitable candidates.
Cost-Effectiveness and Insurance Coverage
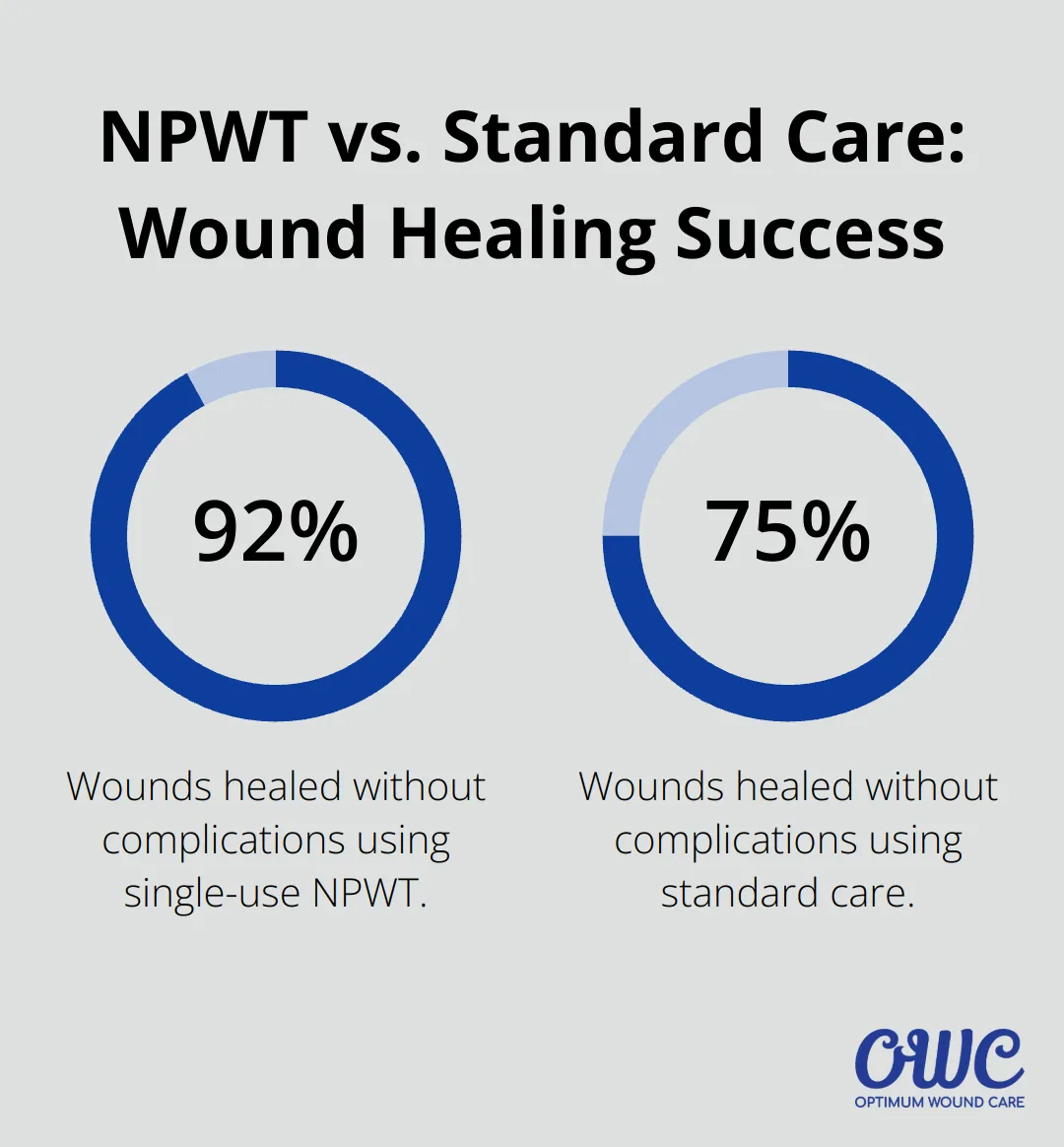
While NPWT may have higher upfront costs than traditional dressings, it often proves cost-effective in the long term. A clinical study reported an increase in wounds that healed without complications: 37/40 (92.5%) in the single-use NPWT group compared to 30/40 (75%) patients in the standard care group. This cost reduction primarily stems from faster healing times and fewer complications.
Most insurance plans (including Medicare) cover NPWT when deemed medically necessary. However, coverage criteria vary, and pre-authorization is often required. Patients should check with their insurance providers before initiating treatment.
Implementation and Monitoring
Proper implementation and monitoring are essential for NPWT success. This includes:
- Thorough wound assessment before treatment
- Appropriate dressing selection and application
- Regular monitoring of wound progress
- Adjustment of therapy settings as needed
Healthcare providers should conduct comprehensive patient education to ensure adherence to treatment protocols and maximize NPWT benefits.
Final Thoughts
Negative pressure therapy has transformed wound management with its proven effectiveness in accelerating healing across various wound types. The evidence strongly supports its superiority over traditional methods in promoting faster closure and reducing complications for conditions ranging from diabetic foot ulcers to surgical incisions. However, NPWT does not serve as a universal solution, and successful outcomes depend on tailoring treatment plans to each patient’s specific needs.
The future of NPWT holds promise, with ongoing research exploring new applications and refining existing techniques. We anticipate advancements in portable devices, smart monitoring systems, and combination therapies that will further enhance the efficacy of negative pressure wound therapy. At OWC Center, we remain committed to evaluating the latest research and incorporating proven innovations into our treatment protocols.
NPWT has already revolutionized wound care, but its full potential remains untapped. As technology progresses and our understanding of wound healing mechanisms deepens, we expect to witness even more impressive results in the coming years. Negative pressure therapy continues to offer hope and healing to patients struggling with complex wounds, solidifying its position as a powerful tool in modern wound management.

