Diabetic Foot Ulcer: Best Wound Care Dressing Options
Diabetic foot ulcers are a serious complication of diabetes that can lead to severe consequences if left untreated. At Swell Country, we understand the critical importance of proper wound care management for these challenging injuries.
In this post, we’ll explore the best diabetic foot ulcer wound care dressing options available today. We’ll guide you through the various types of dressings and help you understand how to choose the right one for optimal healing.
Understanding Diabetic Foot Ulcers
Definition and Prevalence
Diabetic foot ulcers are open sores or wounds that affect people with diabetes. The lifetime risk of foot ulcer is 19% to 34%, and this number is rising with increased longevity and medical complexity of people with diabetes.

Root Causes
The primary factors behind diabetic foot ulcers are neuropathy and peripheral artery disease. Neuropathy (nerve damage) results in a loss of sensation in the feet, causing small injuries or pressure points to go unnoticed and worsen over time. Peripheral artery disease reduces blood flow to the feet, impairing the body’s ability to heal these wounds.
Diabetic neuropathy, particularly complex polyneuropathy, significantly increases the risk of ulceration, infection, and ultimately, amputation.
Risk Factors
Several factors increase the likelihood of developing diabetic foot ulcers:
- Poor glycemic control (HbA1c levels above 7.5%)
- Duration of diabetes (over 10 years)
- Foot deformities
- Previous foot ulceration or amputation
- Obesity
- Smoking
Complications
The complications of diabetic foot ulcers can be severe. Untreated wounds can lead to infections, which may spread to bone or tissue. In extreme cases, amputation becomes necessary. The American Diabetes Association reports that approximately 85% of diabetes-related amputations are preceded by foot ulcers.
Importance of Proper Wound Care
Effective wound care plays a vital role in managing diabetic foot ulcers and preventing complications. A multifaceted approach includes:
- Regular wound assessment and debridement
- Appropriate dressing selection
- Offloading pressure from the wound
- Management of infection and inflammation
- Optimization of blood flow
Research published in the International Journal of Lower Extremity Wounds demonstrates that significantly more ulcers achieved complete healing by 20 weeks in the intervention group than in the group receiving standard care only.
Proper wound care also involves patient education. Healthcare professionals (like those at Optimum Wound Care) teach patients how to perform daily foot checks, maintain good foot hygiene, and recognize early signs of problems. This proactive approach significantly reduces the risk of ulcer development and recurrence.
As we move forward, we’ll explore the various types of wound care dressings available for diabetic foot ulcers, helping you understand the options and their specific benefits in the next section.
Wound Care Dressings for Diabetic Foot Ulcers
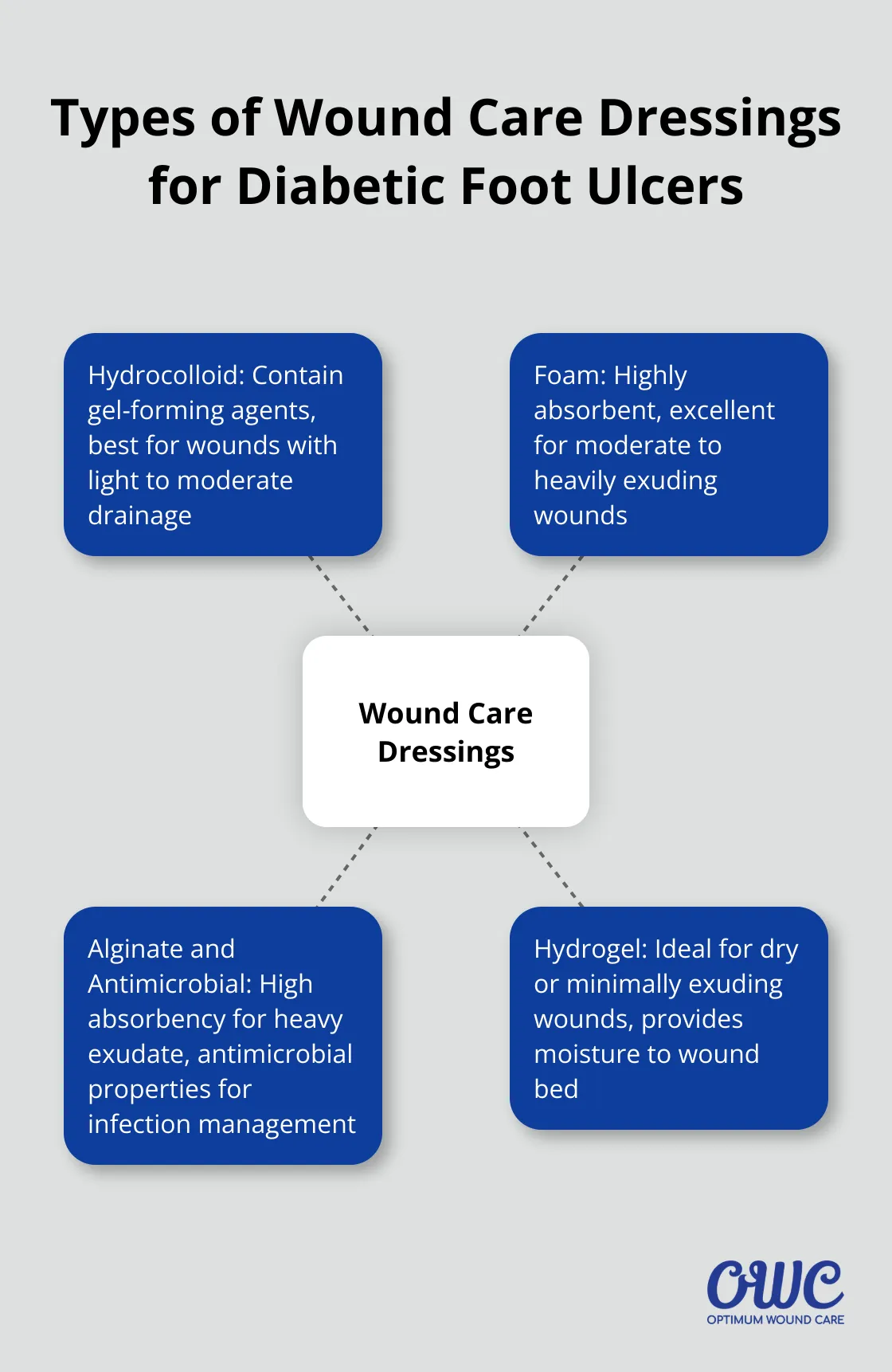
Hydrocolloid Dressings
Hydrocolloid dressings offer versatility for diabetic foot ulcer management. These dressings contain gel-forming agents that interact with wound exudate to create a moist healing environment. They work best for wounds with light to moderate drainage.
Currently there is no research evidence to suggest that any type of hydrocolloid wound dressing is more effective in healing diabetic foot ulcers. However, we advise against using these dressings on infected wounds or those with heavy exudate.
Foam Dressings
Foam dressings provide high absorbency and excellent cushioning for diabetic foot ulcers. They excel in managing moderate to heavily exuding wounds and can remain in place for several days, which reduces dressing change frequency.
Research shows that there is no clear evidence that foam dressings are more effective than other dressings used for management of diabetic foot ulcers. However, their absorbent properties help maintain optimal moisture balance, a key factor in wound healing.
Alginate and Antimicrobial Dressings
Alginate dressings, derived from seaweed, offer high absorbency for wounds with heavy exudate. Upon contact with wound fluid, they form a gel that maintains a moist environment and promotes healing.
Antimicrobial dressings (often containing silver or iodine) play a vital role in managing infected or at-risk diabetic foot ulcers. Silver dressings significantly enhance healing in diabetic foot ulcers but show no marked effect in venous leg ulcers. Silver dressings can accelerate healing in diabetic foot ulcers.
Hydrogel Dressings
Hydrogel dressings excel in treating dry or minimally exuding diabetic foot ulcers. They provide moisture to the wound bed, which promotes autolytic debridement and facilitates necrotic tissue removal. However, we recommend close wound monitoring when using hydrogels, as excessive moisture can lead to maceration of the surrounding skin.
Choosing the Right Dressing
Selecting the appropriate dressing for diabetic foot ulcers requires careful assessment of wound characteristics and patient needs. We emphasize the importance of regular wound evaluation and adjustment of dressing choices as the wound progresses through different healing stages.
In the next section, we’ll explore how to match specific wound characteristics with the most suitable dressing options, ensuring optimal healing outcomes for diabetic foot ulcers.
How to Select the Best Dressing for Diabetic Foot Ulcers
Selecting the right dressing for diabetic foot ulcers can significantly impact wound healing outcomes. At Optimum Wound Care, we provide practical guidance to help you make informed decisions about wound care dressings.
Assess Wound Characteristics
The first step in selecting an appropriate dressing is to thoroughly assess the wound. Key factors to consider include:
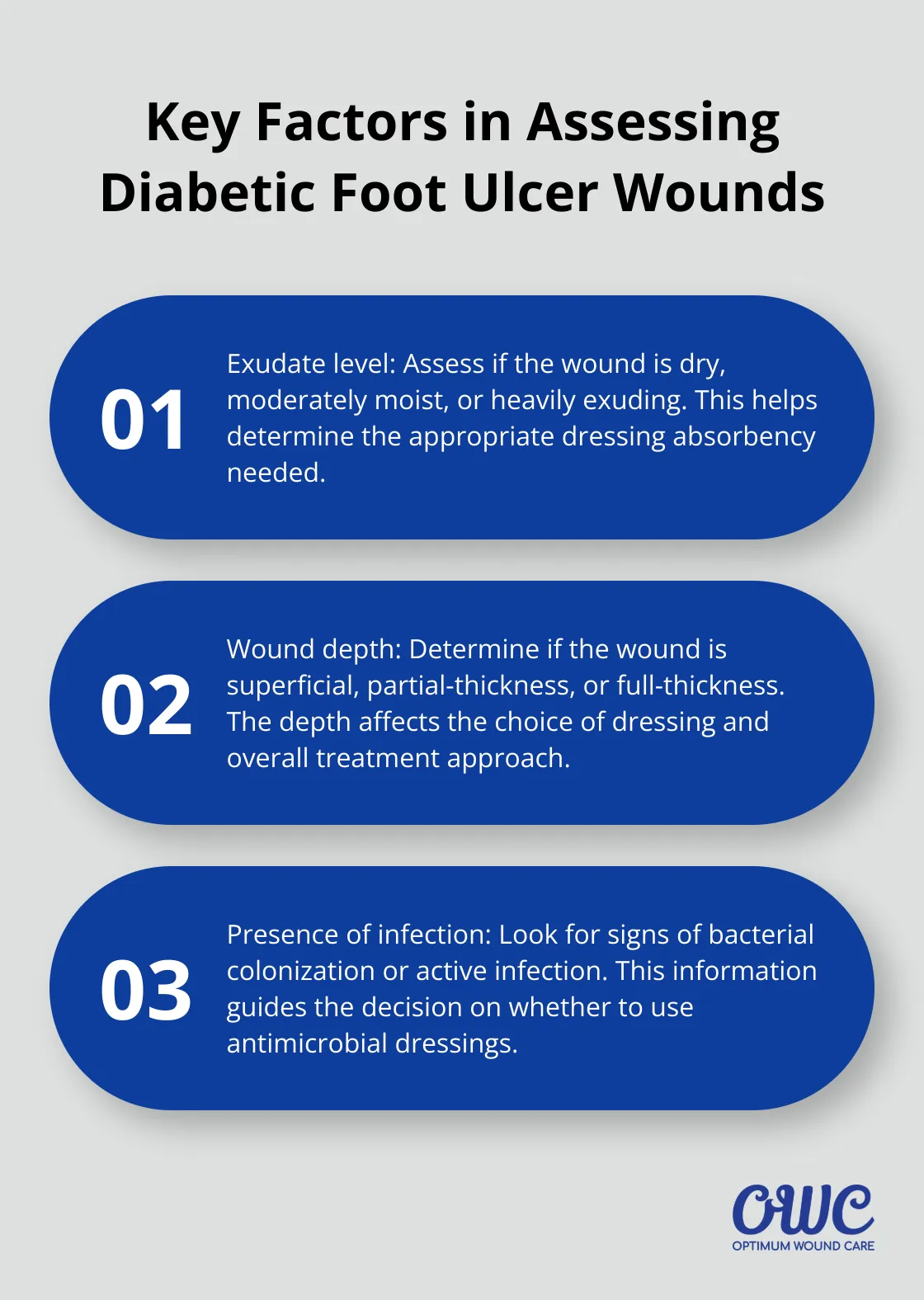
A heavily exuding wound might benefit from an alginate or foam dressing, while a dry wound may require a hydrogel to maintain moisture balance.
Match Dressing Properties to Wound Needs
After assessing the wound, match its characteristics to the properties of available dressings. Here’s a quick guide:
- For heavily exuding wounds: Choose highly absorbent dressings like alginates or foams.
- For dry wounds: Opt for moisture-donating dressings such as hydrogels.
- For infected wounds: Consider antimicrobial dressings containing silver or iodine.
- For wounds with delicate surrounding skin: Use gentle adhesive or non-adherent dressings to prevent further damage.
Maintain Optimal Moisture Balance
Proper moisture balance is essential for wound healing. Too much moisture can lead to maceration, while too little can delay healing. The ideal dressing should:
- Absorb excess exudate without drying out the wound bed
- Maintain a moist environment to promote cell migration and proliferation
- Protect the wound from external contaminants
Delicate control of the wound and surrounding area moisture balance has been proven to accelerate wound healing.
Change Dressings at the Right Time
Proper timing of dressing changes is essential for effective wound management. Generally:
- Change dressings when they’re saturated, loose, or visibly soiled
- Follow manufacturer guidelines for maximum wear time
- Assess the wound at each dressing change for signs of improvement or deterioration
Seek professional help if you notice:
- Increased pain, redness, or swelling around the wound
- Foul odor or increased drainage
- No signs of improvement after 2-4 weeks of treatment
At Optimum Wound Care, we specialize in managing complex diabetic foot ulcers. Our team of experts can provide personalized advice on dressing selection and overall wound management strategies.
Proper dressing selection is just one part of comprehensive diabetic foot ulcer care. Regular wound assessment, offloading, and blood sugar control are equally important for successful healing outcomes.
Final Thoughts
Diabetic foot ulcer wound care dressing selection plays a vital role in the healing process. We match dressing properties to specific wound needs, considering factors such as exudate level, depth, and infection presence. Optimal moisture balance promotes wound healing, and regular assessment allows for timely treatment adjustments.
Effective diabetic foot ulcer management requires a holistic approach. This includes proper offloading, blood sugar control, and patient education alongside appropriate dressing selection. We at Swell Country understand that each diabetic foot ulcer demands personalized care for the best outcomes.
Our team at Optimum Wound Care specializes in treating complex wounds, including diabetic foot ulcers. We use advanced therapies and cutting-edge techniques to speed up recovery and improve quality of life. If you’re dealing with a diabetic foot ulcer, don’t hesitate to seek our expert help for tailored treatment plans and support throughout your healing journey.