How to Care for Diabetic Foot Ulcers Effectively
Diabetic foot ulcers are a serious complication that affects many people with diabetes. These wounds can lead to severe infections, amputations, and a reduced quality of life if not properly managed.
At Optimum Wound Care (OWC), we understand the importance of effective care for diabetic foot ulcers. This blog post will guide you through the essential steps to prevent, treat, and manage these challenging wounds, helping you maintain foot health and overall well-being.
Understanding Diabetic Foot Ulcers
What Are Diabetic Foot Ulcers?
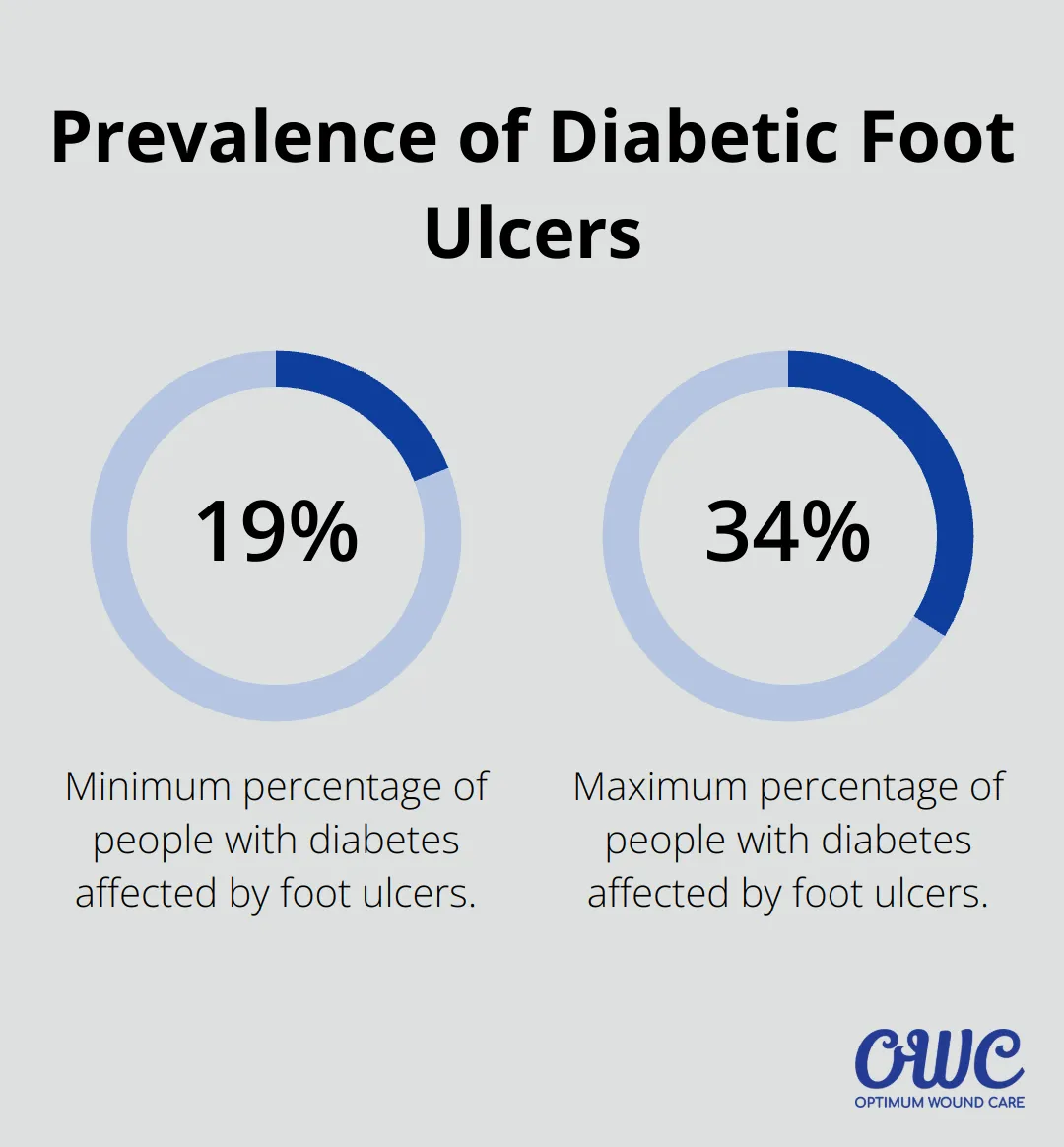
Diabetic foot ulcers are open sores or wounds that affect about 19% to 34% of people with diabetes. These ulcers typically develop on the bottom of the foot, often due to a combination of poor circulation and nerve damage caused by long-term high blood sugar levels.
The Root Causes of Diabetic Foot Ulcers
Two major complications of diabetes primarily cause diabetic foot ulcers: peripheral neuropathy and peripheral arterial disease. Peripheral neuropathy results in a loss of sensation in the feet, making it difficult for patients to feel injuries or pressure points. This lack of sensation can lead to unnoticed cuts, blisters, or other injuries that may develop into ulcers.
Peripheral arterial disease reduces blood flow to the feet. This impaired circulation slows down the healing process and makes the feet more susceptible to infections. A study published in the Journal of Diabetes Research found that up to 50% of people with diabetes may develop peripheral neuropathy, which significantly increases their risk of foot ulcers.
High-Risk Factors for Diabetic Foot Ulcers
Several factors increase the likelihood of developing diabetic foot ulcers. Poor glycemic control tops the list, with studies showing a positive but not significant association between high HbA1c levels and the risk of lower limb ulcers in diabetic patients. Other risk factors include:
- Duration of diabetes (the longer a person has had diabetes, the higher their risk)
- Foot deformities (conditions like bunions or hammertoes can create pressure points)
- Previous foot ulcers or amputations (these indicate a history of foot problems)
- Obesity (excess weight puts additional pressure on the feet)
- Smoking (this habit further reduces blood flow to the extremities)
Common Locations and Types of Diabetic Foot Ulcers
Diabetic foot ulcers most frequently occur on weight-bearing areas of the foot, such as the ball of the foot, the big toe, and the heel. The American Diabetes Association reports that about 85% of diabetic foot ulcers occur on the bottom of the foot.
There are several types of diabetic foot ulcers:
- Neuropathic ulcers: These result from nerve damage and typically occur on pressure points.
- Ischemic ulcers: Poor blood flow causes these ulcers, which often appear on the tips of toes or the edges of the foot.
- Neuro-ischemic ulcers: A combination of nerve damage and poor circulation causes these complex ulcers.
Understanding the type of ulcer is essential for effective treatment. Healthcare professionals conduct thorough assessments to determine the exact nature of each ulcer, allowing them to tailor their treatment approach for optimal healing outcomes.
As we move forward, we’ll explore effective treatment strategies that can help manage these challenging wounds and promote healing. From proper wound cleaning techniques to advanced dressing options, the next section will provide valuable insights into the care of diabetic foot ulcers.
Effective Treatment Strategies for Diabetic Foot Ulcers
Proper Wound Cleaning and Debridement
The cornerstone of diabetic foot ulcer treatment is thorough wound cleaning and debridement. This process eliminates dead tissue and bacteria, which promotes a healthy wound bed essential for healing. Wound care plays a pivotal role in the management of diabetic foot ulcers, which comprises cleaning the wound with normal saline following aseptic techniques.
We recommend the use of sterile saline solution to clean the wound gently. For debridement, sharp debridement performed by a healthcare professional often yields the best results. This technique involves the use of a scalpel or scissors to remove dead tissue with precision. It’s important to have a trained professional perform this procedure to avoid damage to healthy tissue.
Advanced Dressing Options
The selection of an appropriate dressing plays a vital role in optimal wound healing. Modern dressings do more than just cover the wound; they create an ideal environment for healing. However, there is currently no robust evidence for differences between wound dressings for any outcome in foot ulcers in people with diabetes (treated in any setting).
Hydrocolloid dressings prove particularly effective for diabetic foot ulcers. These dressings form a gel when they contact wound exudate, maintaining a moist environment that accelerates healing. For wounds with heavy exudate, alginate dressings excel as they can absorb up to 20 times their weight in fluid.
Offloading Methods
Reducing pressure on the wound, known as offloading, is essential for healing diabetic foot ulcers. Total contact casting is considered the gold standard for offloading, but it requires expertise to apply correctly.
For patients unable to use total contact casting, removable cast walkers or healing sandals are recommended. These devices redistribute pressure away from the ulcer site, allowing for faster healing. Consistent use of these devices, even at home, maximizes their effectiveness.
Negative Pressure Wound Therapy
Negative pressure wound therapy (NPWT) has revolutionized the treatment of diabetic foot ulcers. This technique employs a vacuum dressing to promote healing by increasing blood flow to the wound area and removing excess fluid. Generally speaking, NPWT can help to heal the wound and lower the risk of amputations in people with diabetes.
State-of-the-art NPWT devices are portable and user-friendly, allowing patients to continue treatment at home and reducing the need for frequent clinic visits. However, regular check-ups remain important to ensure the therapy’s effectiveness and make necessary adjustments.
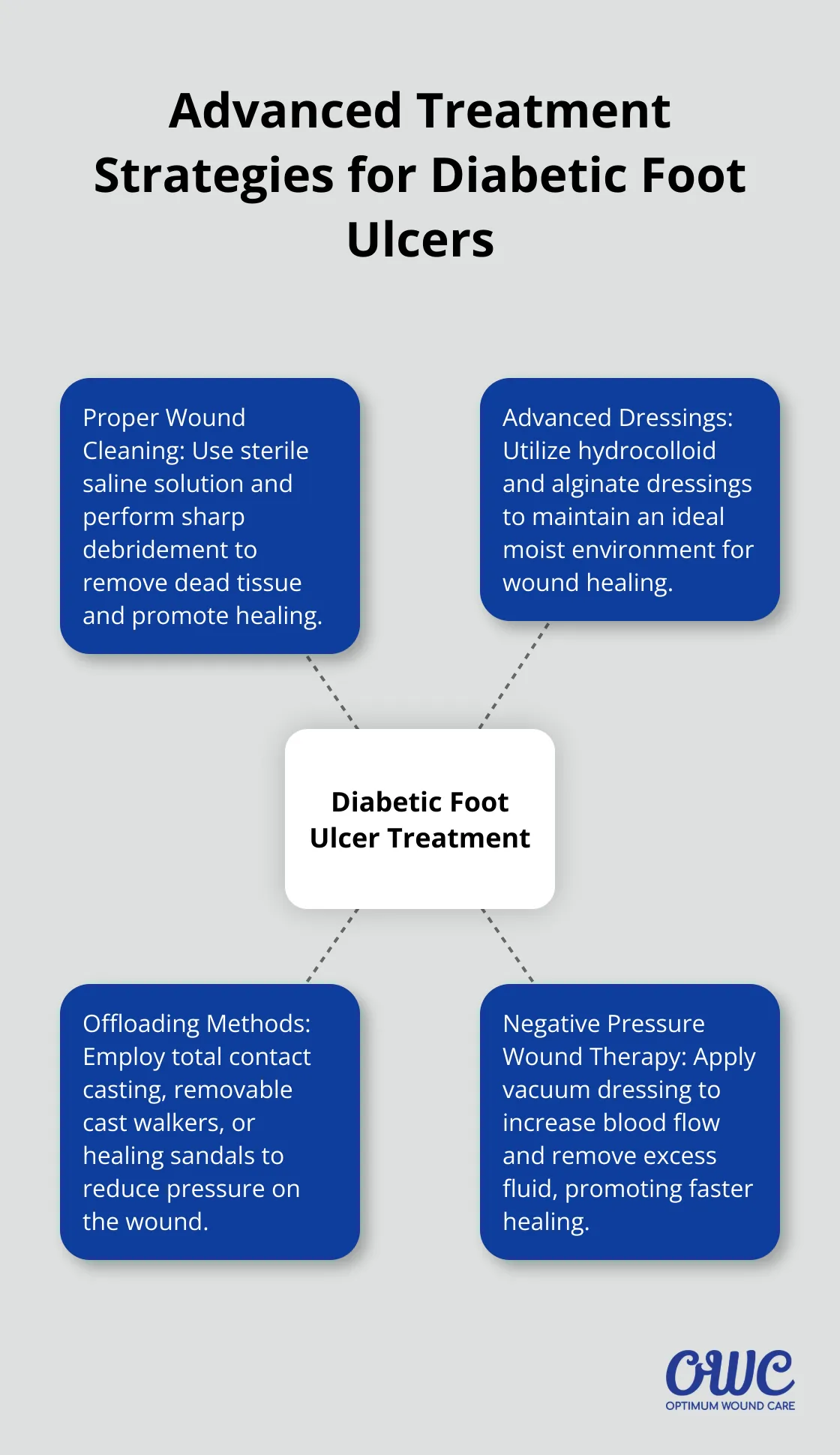
The treatment of diabetic foot ulcers requires a combination of these advanced techniques. As we move forward, we’ll explore how to prevent complications and promote faster healing through lifestyle changes and proper foot care. These strategies complement the treatment methods discussed here, forming a comprehensive approach to diabetic foot ulcer management.
Accelerating Healing and Preventing Complications
Blood Sugar Control for Optimal Healing
Maintaining optimal blood sugar levels is essential for wound healing. High blood glucose impairs the body’s natural healing processes and increases infection risk. A study evaluated the association between hemoglobin A1c (A1C) and wound outcomes in patients with diabetic foot ulcers (DFUs).
To achieve better glycemic control:
- Monitor blood sugar levels regularly (at least 4 times a day)
- Adjust medication as directed by your healthcare provider
- Follow a balanced diet rich in lean proteins, whole grains, and vegetables
- Engage in regular physical activity (as approved by your doctor)
Early Detection and Treatment of Infections
Infection is a major concern in diabetic foot ulcers and can significantly delay healing. The International Working Group on the Diabetic Foot reports that up to 58% of diabetic foot ulcers become infected. Early detection and treatment are vital.
Key signs of infection to watch for:
- Increased redness or warmth around the wound
- Swelling or tenderness
- Foul odor or increased drainage
- Fever or chills
Contact your healthcare provider immediately if you notice any of these signs. Prompt evaluation and treatment of infected wounds prevent further complications.
Nutrition for Wound Healing
Nutrition plays a critical role in wound healing. Current studies have not shown a clear effect of proteins and amino acids in the healing of diabetic foot wounds, but there is some evidence suggesting potential benefits.
Key nutrients for optimal wound healing:
- Protein: Try to consume 1.2-1.5 grams per kilogram of body weight daily
- Vitamin C (supports collagen formation): Found in citrus fruits, berries, and leafy greens
- Zinc (aids in protein synthesis): Found in lean meats, nuts, and seeds
- Vitamin A (supports immune function): Found in sweet potatoes, carrots, and spinach
Consider consulting with a registered dietitian to develop a personalized nutrition plan that supports wound healing while managing blood sugar levels.

Regular Monitoring and Follow-ups
Regular check-ups are essential for tracking progress and adjusting treatment as needed. A study in the International Journal of Lower Extremity Wounds found that patients who had weekly follow-ups had a 52% higher healing rate compared to those with less frequent visits.
We recommend:
- Weekly wound assessments by a healthcare professional
- Regular measurement of wound size and depth
- Adjustment of treatment plans based on healing progress
- Ongoing patient education on proper wound care techniques
Effective management of diabetic foot ulcers requires a multifaceted approach and consistent care. At OWC Center, we provide comprehensive, personalized treatment to help you achieve optimal healing outcomes.
Final Thoughts
Effective care for diabetic foot ulcers demands a comprehensive approach. Proper wound cleaning, advanced dressings, offloading methods, and negative pressure wound therapy all contribute to successful healing. Blood sugar control and early infection detection also play vital roles in preventing complications and promoting faster recovery.
Nutrition and regular monitoring support the healing process of diabetic foot ulcers. A balanced diet rich in proteins, vitamins, and minerals can accelerate wound closure. Frequent check-ups with healthcare professionals allow for timely adjustments to treatment plans and ensure optimal healing outcomes.
Professional help is essential when dealing with diabetic foot ulcers. OWC Center offers specialized wound care services for these challenging conditions. Our team, led by wound care specialist provides personalized treatment to improve your foot health and overall well-being.