How to Treat Diabetic Foot Ulcers Effectively
Diabetic foot ulcers are a serious complication that can lead to severe consequences if left untreated. At OWC Center, we understand the importance of providing the best wound care for diabetic foot ulcers to prevent infections and potential amputations.
In this blog post, we’ll explore effective treatment strategies, preventive measures, and self-care tips to help manage this condition. Our goal is to empower you with practical knowledge to improve your foot health and overall well-being.
What Are Diabetic Foot Ulcers?
Definition and Causes
Diabetic foot ulceration is a devastating complication of diabetes that is associated with infection, amputation, and death. These ulcers can become serious and potentially life-threatening if not treated promptly and effectively. At Optimum Wound Care, we see many patients who struggle with this condition.
The primary causes of diabetic foot ulcers stem from a combination of factors related to diabetes. High blood sugar levels over time can damage nerves (neuropathy) and blood vessels, which leads to reduced sensation and poor circulation in the feet. As a result, small injuries or pressure points can go unnoticed and develop into ulcers.
The lifetime risk of foot ulcer is 19% to 34% in people with diabetes. This statistic highlights the need for vigilant foot care among diabetic patients.

Key Risk Factors
Several factors increase the likelihood of developing diabetic foot ulcers:
- Poor glycemic control: Consistently high blood sugar levels accelerate nerve damage and impair healing.
- Duration of diabetes: The risk increases with the length of time a person has had diabetes. Studies show that patients who’ve had diabetes for over 10 years face a significantly higher risk.
- Foot deformities: Conditions like bunions or hammertoes create pressure points that can lead to ulceration.
- Previous foot ulcers or amputations: A history of these issues increases the risk of future ulcers.
- Peripheral neuropathy: Loss of sensation in the feet can lead to unnoticed injuries.
- Peripheral artery disease: Poor blood flow to the feet impairs healing and increases ulcer risk.
Recognizing Symptoms
Early detection plays a vital role in managing diabetic foot ulcers. Common symptoms include:
- Drainage on socks
- Redness or swelling
- Unusual warmth in a specific area of the foot
- Pain (although some patients may not feel pain due to neuropathy)
Potential Complications
If left untreated, diabetic foot ulcers can lead to severe complications. Hospital admissions for diabetic foot ulcers were relatively stable between 2003 and 2007, ranging from 112,000 to 115,000 admissions per year.
Potential complications include:
- Deep tissue infections
- Osteomyelitis (bone infection)
- Gangrene
- Amputation
At Optimum Wound Care, we emphasize the importance of regular foot checks and immediate attention to any changes or injuries (no matter how small they may seem). Early intervention is key to preventing these serious complications and ensuring the best possible outcomes for our patients.
As we move forward, we’ll explore effective treatment strategies that can help manage diabetic foot ulcers and prevent these complications from occurring.
Effective Treatment Strategies for Diabetic Foot Ulcers
At Optimum Wound Care, we’ve observed how proper treatment can significantly improve outcomes for patients with diabetic foot ulcers. Let’s explore the most effective strategies we use to promote healing and prevent complications.
Wound Cleaning and Debridement
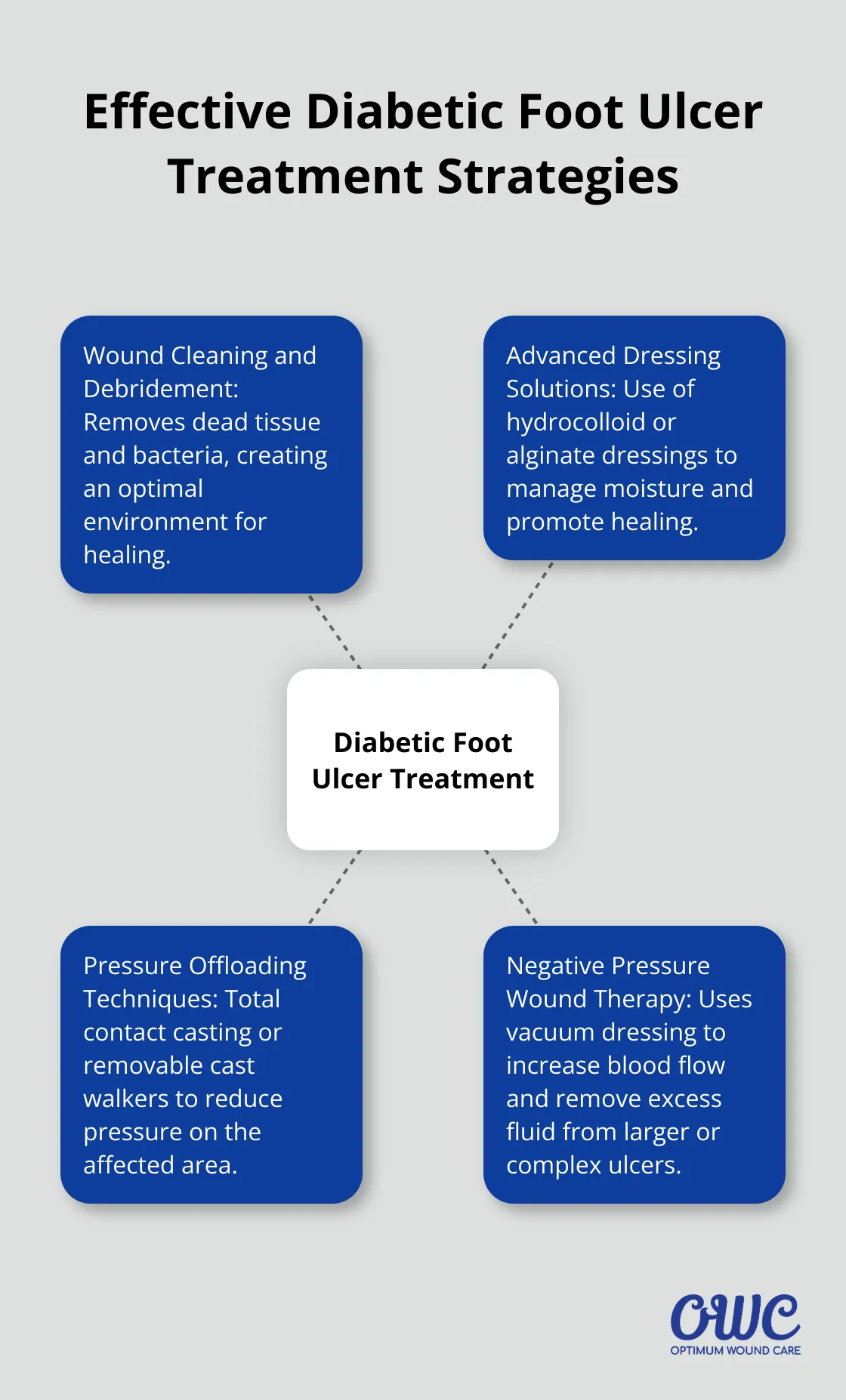
The first step in treating diabetic foot ulcers involves proper cleaning and debridement. This process removes dead tissue and bacteria, creating an optimal environment for healing. Debridement of diabetic foot ulcers is regarded as an intervention that accelerates ulcer healing and may reduce complications including amputations, infections, and poor outcomes.
We employ a combination of techniques, including:
- Sharp debridement with sterile instruments
- Enzymatic debridement using specialized ointments
These methods are tailored to each patient’s needs and the ulcer’s characteristics.
Advanced Dressing Solutions
Selecting the right dressing is essential for ulcer management. We often use hydrocolloid dressings, which create a moist environment that accelerates healing. However, current research does not suggest that any type of hydrocolloid wound dressing is more effective in healing diabetic foot ulcers than other dressing types.
For heavily exuding wounds, we might select alginate dressings, which can absorb up to 20 times their weight in wound fluid. This helps manage moisture and reduces the risk of maceration around the wound edges.
Pressure Offloading Techniques
Reducing pressure on the affected area is vital for healing. Total contact casting (TCC) is one of the methods we use. However, a recent study found that the overall healing rate at 12 weeks was 33% and was not significantly different between various offloading device groups.
For patients who can’t tolerate TCC, we might recommend:
- Removable cast walkers
- Custom-made orthotic devices
These alternatives can help reduce pressure on the ulcer.
Negative Pressure Wound Therapy
For larger or more complex ulcers, we often turn to negative pressure wound therapy (NPWT). This technique uses a vacuum dressing to promote healing by increasing blood flow and removing excess fluid from the wound.
At Optimum Wound Care, we combine these evidence-based treatments with personalized care plans to achieve the best possible outcomes for our patients. Early intervention plays a key role in successful treatment. If you notice any signs of a foot ulcer, seek professional help promptly. Our team stands ready to provide expert care and support throughout your healing journey.
In the next section, we’ll discuss preventive measures and self-care tips that can help you maintain healthy feet and reduce the risk of developing diabetic foot ulcers.
How to Prevent Diabetic Foot Ulcers
At Optimum Wound Care, we believe prevention is the best medicine for diabetic foot ulcers. Here are practical steps you can take to reduce your risk and maintain healthy feet.
Daily Foot Checks: Your First Line of Defense
Examine your feet every day. Look for changes in color, temperature, or sensation. Check between your toes and the soles of your feet for cuts, blisters, or sores. Use a mirror if you have trouble seeing all areas of your feet. Contact your healthcare provider immediately if you notice anything unusual.
Maintain proper foot hygiene. Wash your feet daily with lukewarm water and mild soap. Dry thoroughly, especially between the toes. Apply a moisturizer to prevent dry skin, but avoid putting it between your toes as this can lead to fungal infections.
Blood Sugar Control: The Foundation of Foot Health
Maintain good blood sugar control to prevent diabetic foot ulcers. The American Diabetes Association suggests keeping your A1C below 7% can significantly reduce your risk of developing foot complications. Work with your healthcare team to develop a management plan that includes regular blood sugar monitoring, a balanced diet, and appropriate medication if necessary.
Footwear Matters: Choosing the Right Shoes
Wear shoes that fit well and provide adequate support. Avoid going barefoot, even indoors. When buying new shoes, have your feet measured and try them on later in the day when your feet are slightly swollen.
Consider custom orthotics if you have foot deformities or pressure points. A study published in the Journal of Foot and Ankle Research found that custom-made foot orthoses can significantly reduce peak plantar pressure in people with diabetes (potentially lowering the risk of ulceration).
Lifestyle Changes for Better Foot Health
Quit smoking to improve your foot health. Smoking significantly increases the risk of diabetic foot amputation compared with non-smoking.
Exercise regularly to improve circulation and help manage blood sugar levels. Try to do at least 150 minutes of moderate-intensity aerobic activity per week, as recommended by the Centers for Disease Control and Prevention. However, always consult with your healthcare provider before starting a new exercise regimen (especially if you have existing foot problems).

Final Thoughts
Diabetic foot ulcers require prompt and effective treatment to prevent severe complications. We use strategies like proper cleaning, advanced dressings, pressure offloading, and negative pressure wound therapy to promote healing. Early intervention and consistent care significantly improve outcomes for patients with these challenging wounds.
Specialized clinics offer comprehensive treatment options for those seeking the best wound care for diabetic foot ulcers. Our team uses cutting-edge techniques and personalized treatment plans to address each patient’s unique needs. We combine clinical expertise with compassionate care to help patients heal faster and regain their quality of life.
Prevention remains the most effective approach to managing diabetic foot ulcers. Individuals with diabetes can reduce their risk by implementing self-care tips and working closely with healthcare providers. With the right care and attention, it’s possible to maintain healthy feet despite the challenges of diabetes (including regular foot checks and proper footwear).