What is a Wound VAC for Negative Pressure Therapy?
At Optimum Wound Care (OWC), we’re committed to providing cutting-edge solutions for wound care.
Wound VAC negative pressure therapy has revolutionized the treatment of complex wounds. This innovative approach uses controlled suction to promote faster healing and reduce infection risks.
In this post, we’ll explore how Wound VAC works, its benefits, and proper application techniques to maximize its effectiveness in patient care.
What is a Wound VAC for Negative Pressure Therapy?
Definition and Components
A Wound VAC (Vacuum-Assisted Closure) is a revolutionary technology in wound care. This innovative therapy uses controlled suction to promote faster healing and reduce infection risks. The Wound VAC system consists of three main components:
- A foam dressing
- An adhesive drape
- A pump that creates negative pressure
This setup transforms wound healing by actively promoting tissue regeneration and reducing complications.
The Science Behind Negative Pressure Therapy
The effectiveness of Wound VAC lies in its use of sub-atmospheric pressure. When applied to a wound, it creates negative pressure to help reduce complications and optimize wound healing. This negative pressure produces several beneficial effects:
- It extracts excess fluid from the wound, which reduces swelling and infection risk.
- It boosts blood flow to the wound area, delivering more oxygen and nutrients to support healing.
- It draws the wound edges together, which accelerates closure.
- It encourages the formation of new tissue (granulation tissue).
Research indicates that Wound VAC can significantly improve healing times. A study found that median time to complete wound healing was 21 days with VAC therapy compared to 34 days with conventional treatment.

Suitable Wound Types
Wound VAC therapy proves effective for various types of wounds, including:
- Diabetic foot ulcers
- Pressure ulcers
- Surgical wounds that have opened (dehisced)
- Traumatic wounds
- Skin grafts
However, Wound VAC isn’t appropriate for all wound types. It should not be used on wounds with exposed organs, untreated osteomyelitis, or malignancy. A thorough assessment by a wound care specialist determines if Wound VAC is the right choice for each case.
The Application Process
Applying a Wound VAC requires expertise and precision. The process involves these steps:
- The wound is thoroughly cleaned and debrided.
- The foam dressing is cut to fit the wound precisely.
- The adhesive drape is applied, ensuring a perfect seal around the wound.
- The tubing is connected to the vacuum pump and the system is activated.
Typically, the dressing is changed every 48 to 72 hours. This schedule allows for optimal healing while minimizing disruption to the wound bed.
Wound VAC represents a significant advancement in wound care. Its ability to accelerate healing and reduce complications makes it an invaluable tool in modern wound management. As we move forward, let’s explore the specific benefits and advantages that Wound VAC treatment offers to patients.
Benefits and Advantages of Wound VAC Treatment
Accelerated Healing Process
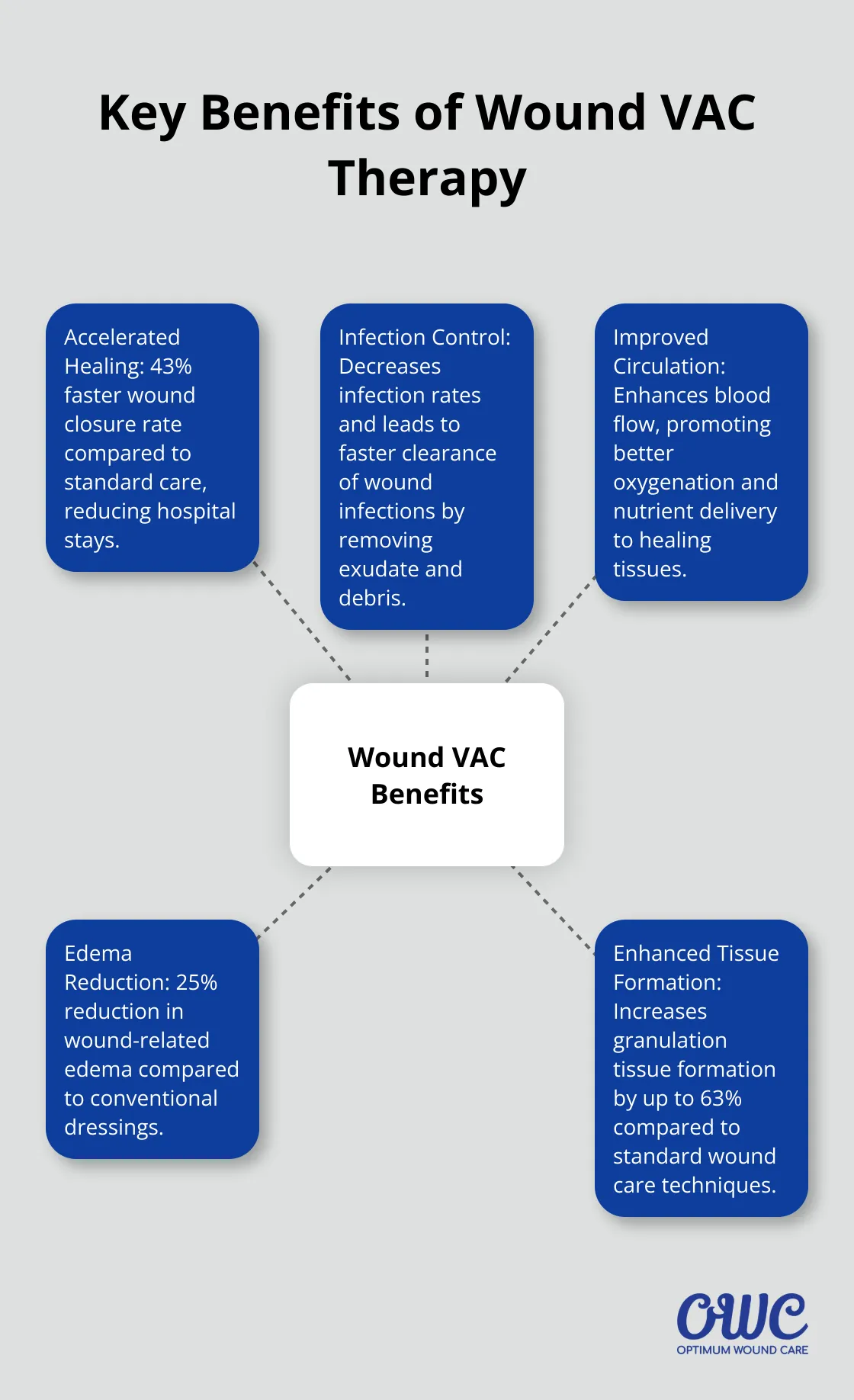
Wound VAC therapy significantly speeds up the healing process. A study published in the Journal of Wound Care found that patients treated with negative pressure wound therapy experienced a 43% faster wound closure rate compared to those receiving standard care. This acceleration in healing can mean fewer hospital stays and a quicker return to normal activities for patients.
Infection Control
One of the most significant benefits of Wound VAC is its ability to reduce infection risks. The constant removal of wound exudate and debris creates an environment less conducive to bacterial growth. Research shows that Wound VAC therapy can decrease infection rates in certain types of wounds compared to conventional therapy, and lead to faster clearance of wound infections.
Improved Circulation and Edema Reduction
Wound VAC therapy enhances blood flow to the wound area, which promotes better oxygenation and nutrient delivery to healing tissues. This improved circulation also helps reduce edema, a common complication in wound healing. A study in the International Wound Journal reported a 25% reduction in wound-related edema with Wound VAC treatment compared to conventional dressings.
Enhanced Tissue Formation
The negative pressure applied by Wound VAC stimulates the formation of granulation tissue, which plays a vital role in wound healing. This effect particularly benefits deep or complex wounds. Data from the Journal of Plastic, Reconstructive & Aesthetic Surgery indicates that Wound VAC can increase granulation tissue formation by up to 63% compared to standard wound care techniques (an impressive boost to the healing process).
Customized Treatment Approach
At Optimum Wound Care, we integrate Wound VAC therapy into our comprehensive wound management approach. Our experienced team, led by Wound/Ostomy Specialist Mosayeb “Moe” Karimi, MSN, FNP, WOC, carefully assesses each patient to determine if Wound VAC is the right choice for their specific condition. This personalized approach ensures that patients receive the most effective treatment for their unique wound healing needs.
The numerous benefits of Wound VAC therapy highlight its importance in modern wound care. However, to maximize these advantages, proper application and management are essential. In the next section, we will explore the specifics of how to apply and manage a Wound VAC system effectively, ensuring optimal results for patients.
How to Apply and Manage Wound VAC Effectively
Precise Application Procedure
Wound VAC application demands attention to detail and sterile technique. A healthcare provider will cover your wound with a foam or gauze wound dressing. An adhesive film will be put over the dressing and wound. This seals the wound.
Optimal Dressing Change Frequency
The frequency of dressing changes impacts healing significantly. A study found that a 7-day interval between changes of the NPWT is acceptable, considering patient comfort, costs related to the NPWT, and the final flap results.
Fine-Tuning Negative Pressure Levels
The negative pressure level is a key factor in Wound VAC therapy effectiveness. Studies have shown that rate of granulation tissue formation is twice with intermittent negative pressure compared with continuous negative pressure. However, the optimal pressure can vary depending on the wound type and patient tolerance.
We start with a standard pressure of -125 mmHg and adjust based on wound response and patient comfort. Our team monitors the amount of exudate collected and the appearance of the wound to determine if pressure adjustments are necessary.

Addressing Potential Complications
While Wound VAC therapy is generally safe, complications can occur. The most common issues include pain, skin irritation around the wound, and bleeding. To mitigate these risks, we take several precautions:
- Pain management: We use appropriate pain medication and adjust pressure settings if discomfort persists.
- Skin protection: Application of skin barrier products around the wound helps prevent irritation from the adhesive drape.
- Bleeding prevention: For patients on anticoagulants (or with friable tissue), we may use a non-adherent layer between the foam and the wound bed.
In rare cases, more serious complications like infection or fistula formation can occur. Our team conducts regular assessments to catch and address any issues early. We maintain open communication with patients, educating them on signs to watch for and when to contact us immediately.
Final Thoughts
Wound VAC negative pressure therapy revolutionizes modern wound care practices. This innovative approach accelerates healing, reduces infection risks, and improves overall patient outcomes. The therapy enhances blood flow, stimulates tissue growth, and manages wound exudate effectively.
Proper application and management of Wound VAC systems maximize their effectiveness. Healthcare providers must apply dressings precisely, monitor regularly, and adjust negative pressure levels as needed. Addressing potential complications promptly allows practitioners to harness the full potential of this therapy.
At Optimum Wound Care (OWC), we integrate advanced treatments like Wound VAC into comprehensive care plans. Our team strives to accelerate healing, reduce complications, and improve patients’ quality of life (using cutting-edge techniques). We anticipate even greater advancements in negative pressure wound therapy, further enhancing our ability to provide optimal care for challenging wounds.