Diabetic Foot Ulcers: Causes, Prevention, and How OWC Center Can Help
Diabetic foot ulcers are a serious complication affecting millions of people with diabetes worldwide. These painful and potentially dangerous wounds can lead to severe infections and, in extreme cases, amputations.
Understanding Diabetic Foot Ulcers
Definition and Prevalence
Diabetic foot ulcers are open sores or wounds that affect approximately 19% to 34% of people with diabetes during their lifetime. These ulcers typically form on the bottom of the foot, often under the big toe or on the balls of the feet. They pose a serious complication that can lead to infection and, in severe cases, amputation.

The Diabetes-Ulcer Connection
Diabetes contributes to foot ulcer development through several mechanisms:
- Nerve Damage (Neuropathy): High blood sugar levels can damage nerves, resulting in a loss of sensation in the feet. This makes it difficult for patients to feel injuries or pressure points. A study in the New England Journal of Medicine reports that the incidence of neuropathy is associated with potentially modifiable cardiovascular risk factors.
- Poor Circulation: This common issue in diabetes slows down the healing process, making even small wounds more likely to become ulcers. About 130,000 people with diabetes have amputations each year, largely due to foot ulcers.
Identifying Diabetic Foot Ulcers
Diabetic foot ulcers often start as small blisters, cuts, or areas of redness. They frequently appear on weight-bearing areas of the foot (such as the ball of the foot or the bottom of the big toe). However, they can occur anywhere on the foot, including the sides and heel.
One of the most concerning aspects of these ulcers is that they can develop and worsen without causing pain, due to the nerve damage associated with diabetes. This lack of pain can lead to delayed treatment, making regular foot inspections essential for early detection.
Risk Factors for Diabetic Foot Ulcers
Several factors increase the risk of developing diabetic foot ulcers:
- Poor blood sugar control
- Smoking
- Obesity
- Wearing ill-fitting shoes
- Previous foot ulceration or amputation
- End-stage renal disease
- Peripheral neuropathy
The International Working Group on the Diabetic Foot identified the last three factors as the strongest predictors for future diabetic foot ulcers.
Prevention Strategies
Prevention plays a key role in managing diabetic foot ulcers. Effective strategies include:
- Maintaining good blood sugar control
- Performing daily foot inspections
- Wearing proper footwear
- Seeking immediate care for any foot injuries (no matter how minor they may seem)
- Scheduling regular podiatric check-ups
Professional examinations can detect issues before they become serious problems. These preventive measures form the foundation of effective diabetic foot care and can significantly reduce the risk of ulcer development.
As we move forward, we’ll explore specific prevention strategies in more detail, providing practical tips to help individuals with diabetes protect their feet and maintain overall foot health.
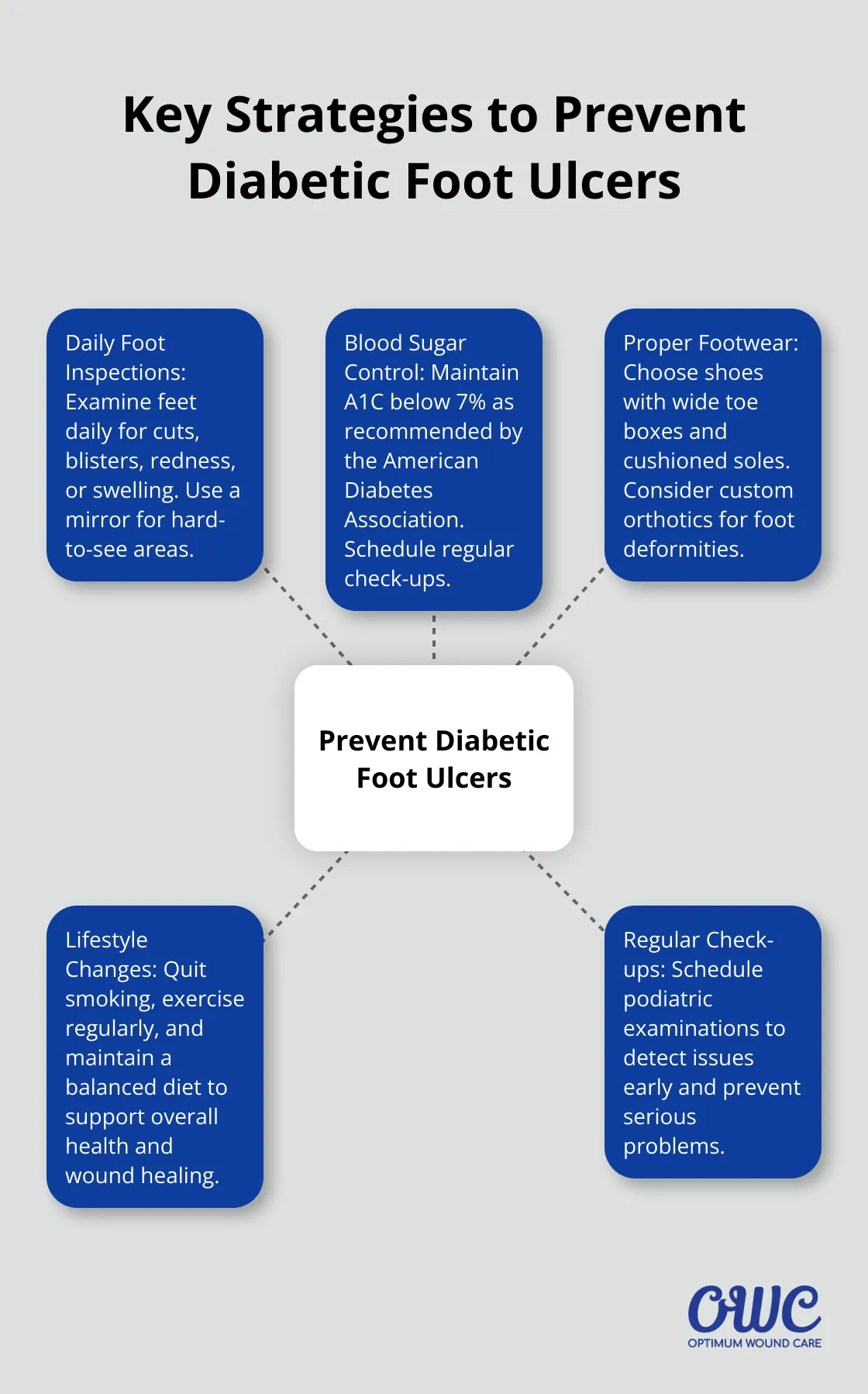
How to Prevent Diabetic Foot Ulcers
Daily Foot Inspections: Your First Line of Defense
Examine your feet every day. Look for cuts, blisters, redness, swelling, or nail problems. Use a mirror to check the bottoms of your feet or ask a family member for help if you have trouble seeing them. The lifetime risk of foot ulcer is 19% to 34% for people with diabetes, and this number is rising with increased longevity and medical complexity.
Practice proper hygiene. Wash your feet daily with lukewarm water and mild soap, but avoid soaking them as this can dry out your skin. After washing, dry your feet thoroughly, especially between the toes where moisture can lead to fungal infections.
Blood Sugar Control: The Foundation of Prevention
Maintain good blood sugar control to prevent diabetic foot ulcers. High blood sugar levels can damage nerves and blood vessels, which increases the risk of foot problems. The American Diabetes Association recommends keeping your A1C below 7%. Schedule regular check-ups with your healthcare provider to stay on track with your blood sugar management.
Footwear Matters: Choose Wisely
Select proper footwear to prevent diabetic foot ulcers. Shoes that fit well and provide adequate support can significantly reduce the risk of foot injuries. Look for shoes with a wide toe box, cushioned soles, and breathable materials.
Consider custom orthotics if you have foot deformities or previous ulcers. These can help distribute pressure evenly across your feet, reducing the risk of ulcer formation. Innovative intelligent insole systems have shown promise in reducing diabetic foot ulcer recurrence at plantar sites.
Lifestyle Changes: Small Steps, Big Impact
Quit smoking to improve your foot health. Smoking narrows blood vessels, reducing circulation to your feet. A study in the New England Journal of Medicine found that smokers with diabetes have a 25% higher risk of developing foot ulcers compared to non-smokers.
Exercise regularly to improve circulation and control blood sugar levels. Try to engage in at least 30 minutes of moderate activity most days of the week. Swimming and cycling are excellent low-impact options that don’t put excessive pressure on your feet.
Eat a balanced diet to support overall health and wound healing. Focus on whole grains, lean proteins, fruits, and vegetables. The American Diabetes Association recommends working with a registered dietitian to create a meal plan that suits your individual needs.
Preventing diabetic foot ulcers requires a comprehensive approach. A team of specialists (like those at OWC Center) can provide personalized guidance and support to help you implement these prevention strategies effectively. Early intervention plays a key role in managing foot health for individuals with diabetes. In the next section, we’ll explore how specialized wound care centers can assist in treating diabetic foot ulcers when prevention isn’t enough.
How OWC Center Treats Diabetic Foot Ulcers
Personalized Assessment and Treatment Plans
OWC Center takes a comprehensive approach to treating diabetic foot ulcers. Our team, led by Family Nurse Practitioner and Wound/Ostomy Specialist Mosayeb “Moe” Karimi, MSN, FNP, WOC, combines clinical expertise with advanced wound care techniques to deliver personalized, effective treatment.
When a patient arrives at OWC Center with a diabetic foot ulcer, we conduct a thorough assessment. We examine the wound, evaluate the patient’s overall health, and consider factors like diabetes control, wound care, infection control, pressure relief, and blood flow optimization. This comprehensive evaluation allows us to create a tailored treatment plan that addresses not just the ulcer, but also the underlying factors contributing to its development.
Our treatment plans often include a combination of wound care techniques. We might use debridement to remove dead tissue and promote healing, followed by the application of specialized dressings that create an optimal healing environment. In some cases, we recommend negative-pressure wound therapy, which has shown consistent benefits compared to control treatments for diabetic foot ulcers.

Advanced Wound Care Techniques
OWC Center stays at the forefront of wound care technology. One of our most effective treatments for diabetic foot ulcers is debridement. This process removes dead or infected tissue from the wound, which promotes healing. Regular debridement is regarded as an effective intervention to accelerate ulcer healing and decrease the risk of serious complications.
We also use a variety of specialized dressings, each designed to address specific aspects of wound healing. Some dressings maintain a moist wound environment (which speeds up healing), while others contain antimicrobial agents to prevent infection (a common complication in diabetic foot ulcers).
Collaborative Care for Comprehensive Management
Treating diabetic foot ulcers effectively requires more than just wound care. We collaborate closely with diabetes management specialists. This team approach ensures that we treat not just the ulcer, but also address the underlying diabetes management issues that may have contributed to its development.
We might work with an endocrinologist to improve a patient’s diabetes control (which is essential for wound healing). Or we might consult with a vascular specialist if poor circulation impedes the healing process. This collaborative approach allows us to provide truly comprehensive care.
Patient Education and Long-Term Support
OWC Center believes that patient education is key to successful treatment and prevention of diabetic foot ulcers. We teach our patients proper foot care techniques, including daily foot inspections and proper hygiene practices. We also educate patients on the importance of good diabetes management and how it relates to foot health.
Our support doesn’t end when the ulcer heals. We provide ongoing care and follow-up to prevent recurrence (which is a significant risk for patients who have had a diabetic foot ulcer). This long-term approach helps our patients maintain their foot health and overall quality of life.
Final Thoughts
Diabetic foot ulcers significantly impact the quality of life for individuals with diabetes. Early intervention and prevention play a vital role in effective management of this condition. OWC Center offers expert care to help patients heal and prevent recurrence of these challenging wounds.
Our team of specialists combines clinical expertise with advanced wound care techniques to deliver personalized, effective diabetic foot ulcer treatment plans. We use state-of-the-art therapies such as debridement, specialized dressings, and negative-pressure wound therapy to promote optimal healing. Our comprehensive approach includes thorough assessments, tailored treatment plans, and ongoing patient education.
We urge individuals with diabetes, especially those at high risk for foot ulcers, to seek professional care at OWC Center.